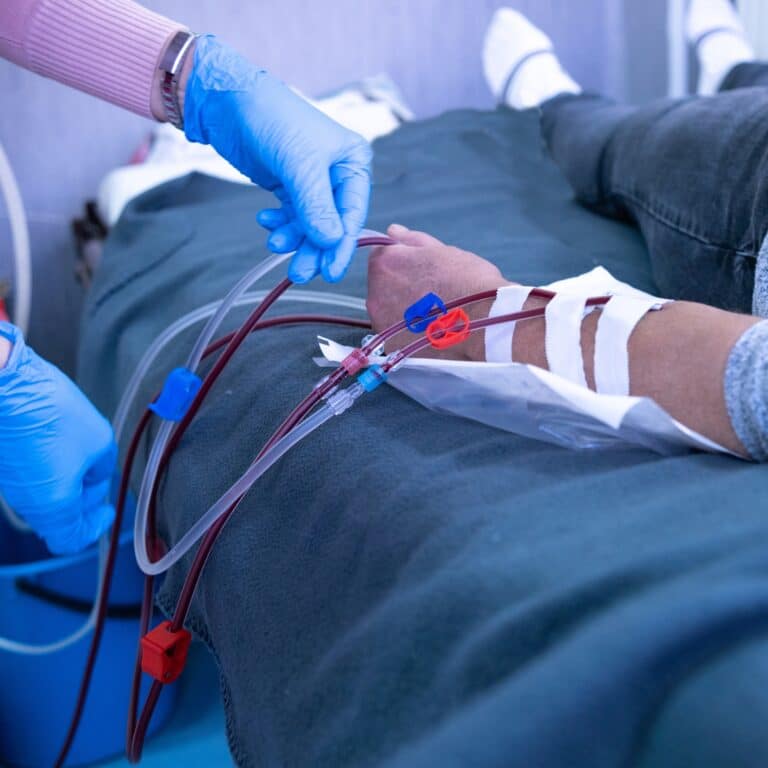
Questions For Your Nephrologist
If you are living with chronic kidney disease (CKD), you understand the importance of managing your condition to maintain your health and quality of life. One significant aspect of managing CKD is building a strong relationship with your nephrologist, who can help guide you through the stages of the disease and develop personalized treatment plans.
Knowing what questions to ask your nephrologist can make all the difference in taking control of your health and making informed decisions about your care planning.
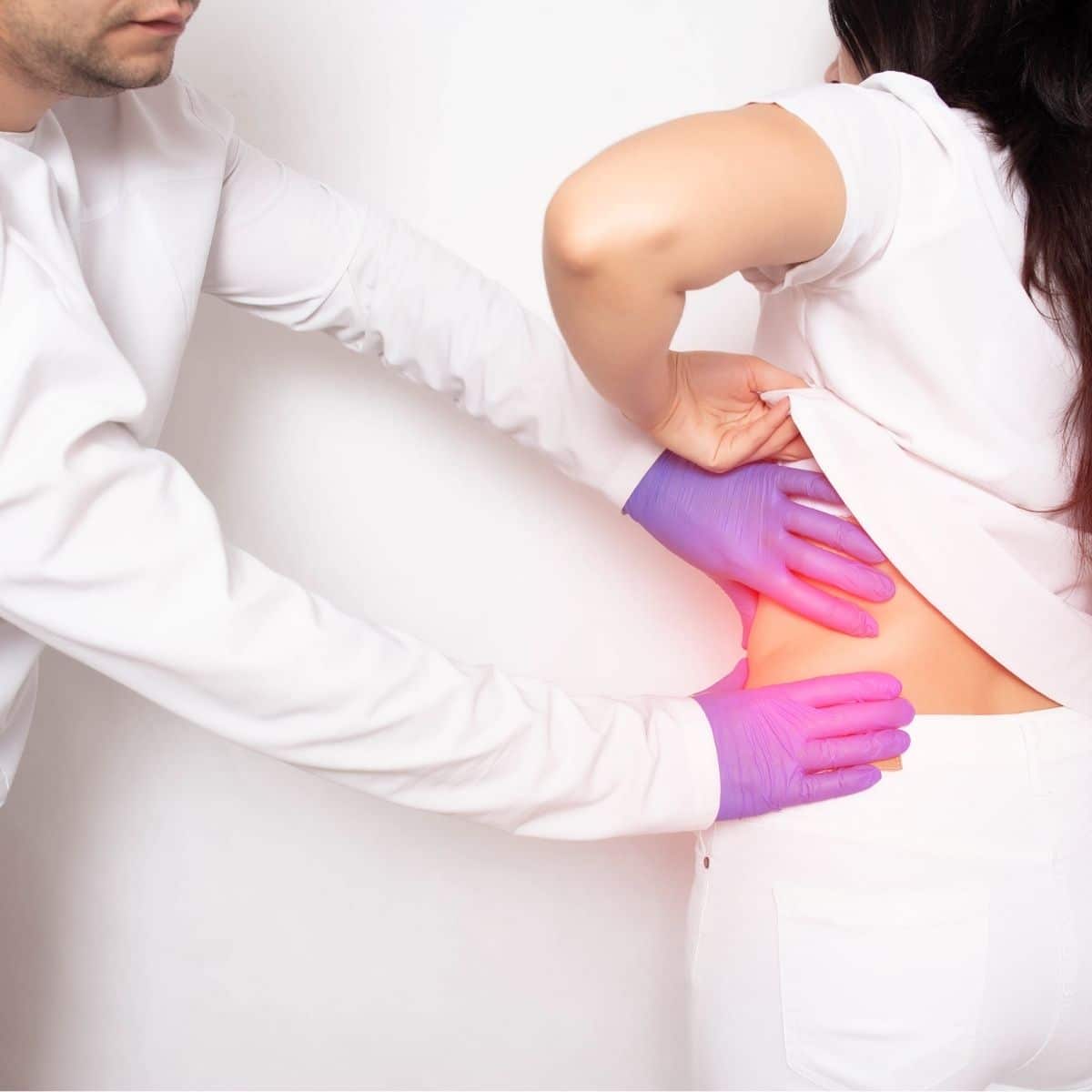
In this article, we will explore the importance of asking questions about early and late-stage CKD, understanding different dietary goals, and finding personalized treatment options. We will delve into topics such as symptoms and causes of CKD (signs and symptoms of kidney failure), potential treatments, and how education and involvement play vital roles in managing your condition.
With knowledge comes power - by asking the right questions during appointments with your nephrologist, you can become an active participant in managing your CKD to achieve better health outcomes. Learn about the qualifications of a nephrologist.
Jump to:
- Key Takeaways
- Preparing for Referral
- CKD Symptoms and Causes
- Importance of Seeing a Nephrologist
- Questions for Early Stage CKD
- Questions for Late Stage CKD
- Renal Dietitian Questions
- Understanding the 5 Stages of CKD
- Personalized Treatment and Care Planning
- Potential Treatment Options
- Importance of Education and Involvement
- Your Nephrologist Is Your Best Resource If You Have CKD
Key Takeaways
- Asking questions about food is crucial after being diagnosed with chronic kidney disease.
- Finding a professional nutritionist and resources for kidney disease-friendly recipes is recommended.
- Support from a family member or friend is important when preparing for a referral to a nephrologist.
- Educate yourself about options and involve a team of trusted friends, family, and nephrologist in decision-making.
Preparing for Referral
Are you feeling overwhelmed about preparing for a referral to a nephrologist? Don't worry, taking the time to organize your questions and concerns, along with bringing necessary information and items, can help ease any anxieties and set you on the path towards personalized treatment and involvement in care planning.
Start by enlisting the support of a family member or friend to accompany you to the appointment. Having someone there for emotional support can make all the difference.
Next, gather all important medical history including a list of symptoms, doctors, medications, insurance cards, and surgery list. Additionally, bring any relevant diagnostic tests such as lab work or blood pressure cuff readings. It's important to arrive 15 minutes early so that you have enough time to fill out paperwork and find parking if needed.
Being prepared ahead of time will help maximize your appointment time with the nephrologist. It's beneficial to come up with a list of questions beforehand so that nothing gets forgotten during the appointment.
Make sure to ask about lifestyle changes that may be necessary as well as what stage of kidney disease you're currently in. Write down any concerns or side effects from current treatments so that they can be addressed during your visit.
Remember, being proactive about your health is one key way to ensure positive outcomes in chronic kidney disease management.
For More Recipes and Ideas --->> Get Your Free Meals and Recipes That Are Perfect for Pre-Dialysis Diets, Pre-Dialysis with Diabetes, or Dialysis Diets.
CKD Symptoms and Causes
Experiencing fatigue, swelling in the legs, and frequent urination may signal the presence of chronic kidney disease. It's important to note that underlying health conditions such as high blood pressure or diabetes can contribute to its development.
Other symptoms include nausea, vomiting, loss of appetite, and difficulty sleeping. The causes of chronic kidney disease may vary, but some common factors include high blood pressure and diabetes. These conditions put a strain on the kidneys over time and can lead to damage.
Other causes include infections, inflammation, obstructions in the urinary tract, and genetic predisposition. Having biological family history of renal disease especially heritable ones like cystic kidney disease and other related medical conditions increases your risk for CKD.
Prevention and management of chronic kidney disease involves addressing its underlying causes as well as making lifestyle changes. This includes maintaining a healthy diet that is low in sodium and protein while also monitoring potassium and phosphorus intake.
Additionally, regular exercise and avoiding smoking are recommended for overall health. Consultation with a nephrologist or renal dietitian can provide more specific guidance on how to manage chronic kidney disease through dietary changes.

Importance of Seeing a Nephrologist
Visiting a nephrologist is crucial for managing chronic kidney disease and understanding the best treatment options available. Here are three reasons why seeing a nephrologist is important:
- Diagnosis: A nephrologist has specialized training and expertise in diagnosing kidney diseases, including chronic kidney disease. They can accurately assess the stage of your CKD, which affects treatment options and progression monitoring. With their help, you can develop a personalized care plan (following a pre-dialysis renal diet) that addresses your specific needs.
- Treatment: Nephrologists are also knowledgeable about the latest treatments for CKD, such as medications to control blood pressure and manage diabetes. They can guide you through lifestyle changes that may be necessary, such as reducing sodium intake or increasing physical activity. By working with a nephrologist, you can slow or halt the progression of CKD and avoid end-stage renal failure (define end stage renal disease).
- Monitoring: Regular monitoring by a nephrologist is crucial for managing CKD effectively. They will monitor your kidney function through blood tests and urine samples to identify any changes or common complications early on. With their guidance, you can make informed decisions about adjusting your treatment plan as needed.
Seeing a nephrologist is essential for anyone with chronic kidney disease. Their expertise in diagnosis, treatment, and monitoring can help you manage the condition effectively and improve your quality of life over time. Don't hesitate to ask questions during your appointment and take an active role in planning your care with their guidance.
Questions for Early Stage CKD
Understanding the causes, signs/symptoms, and dietary changes necessary for early stage CKD can empower individuals to take control of their health and potentially slow or reverse the decline in kidney function. When meeting with your nephrologist for the first time, it's important to ask about these topics.
Ask about what caused your CKD and if there are any underlying conditions contributing to it. Symptoms may not be apparent at this stage, but ask about any warning signs you should watch for (common symptoms of CKD).
Your diet plays a significant role in managing early stage CKD, so ask your nephrologist about necessary dietary changes. They may recommend limiting sodium intake and protein consumption while incorporating more plant-based options into your meals.
A professional nutritionist can provide resources and guidance on creating a kidney-friendly meal plan that works for you. Don't forget to ask about incorporating some of your favorite foods into your diet while still maintaining proper nutrition.
It's essential to take an active role in managing your early stage CKD by asking questions during appointments with healthcare professionals. Understanding the cause of your condition, potential symptoms to look out for, and necessary dietary changes will help you make informed decisions about managing your health effectively.
Questions for Late Stage CKD
When CKD progresses to its later stages, it's essential to have thorough discussions with your healthcare professionals. You should ask about monitoring for health conditions and potential treatments for ESRD like dialysis or kidney transplant.
Additionally, counseling options should be explored as these can help you cope with the emotional burden of living with chronic kidney disease.
To evoke an emotional response in you, here are three sub-lists of questions that could be asked during your appointment:
- Monitoring Symptoms: What symptoms may occur during late-stage CKD? How often should I monitor my blood pressure, weight, and fluid intake? What signs indicate I need urgent medical attention?
- Personalized Care Planning: Is there a care plan specific to my stage of CKD? How can I continue living as independently as possible while receiving treatment? Are there any resources available to manage the financial impact of treating this condition?
- Treatment Options: Can you explain what ESRD treatments (ESRD treatments) entail and how they differ from dialysis? Are there any clinical trials or experimental treatments available for me? Should I consider a kidney transplant, and if so, what are the risks involved? Questions about kidney transplant?
Regarding your treatment considerations, dialysis access may also be a topic of interest if hemodialysis is being considered for you. You may also be offered the option of peritoneal dialysis or renal transplantation. In any case, it’s important to have your kidney doctor discuss all the benefits and risks of complications of each type of treatment with you.
Remember that these questions only scratch the surface of what discussions could occur. It's crucial to involve yourself in your care planning fully by asking thoughtful questions and working closely with your healthcare team. By doing so, you'll be better equipped to make informed decisions about managing your condition.
Discussing late-stage CKD with your nephrologist is vital for managing this chronic illness effectively. Ensure that you understand how best to monitor symptoms and explore personalized care plans tailored specifically for you.
Renal Dietitian Questions
Now that you've discussed late-stage CKD with your nephrologist, it's time to bring up questions for the renal dietitian. This is an essential step in managing your condition since what you eat has a significant impact on your kidneys.
Your renal dietitian can help you set dietary goals and provide tips on how to incorporate your favorite foods into a kidney-friendly diet. One concern many people have after being diagnosed with CKD is dining out at restaurants.
Ask your renal dietitian about kidney-friendly restaurants in your area and how to choose healthy options when eating out. They can also suggest on-the-go snack options that fit within your dietary restrictions.
What you eat has a huge impact on chronic kidney disease, so many of the questions you should consider asking your renal dietitian and your nephrologist should start with what you can do about food.
Here are some questions to get you started:
- How is chronic kidney disease affected by food?
- How much difference can I make with my kidney disease by making dietary changes?
- What are the foods that I should avoid completely?
- What are the foods that I should eat only in moderation, and how often can I make that?
- What is the deal with chronic kidney disease and sodium?
- What are some ways I can cut sodium out of my diet?
- Is there anything else I should avoid at this particular stage of chronic kidney disease?
- Do I need to limit my protein intake?
- Do I need to monitor my potassium or phosphorus intake?
- What foods are high in potassium or phosphorus?
- With the right dietary changes, can I avoid end stage renal failure?
- What are the steps I need to take to slow the progression of my chronic kidney disease?
- What are the benefits of a plant based diet?
- Do I need to limit how much fruit I eat?
- What are some resources (books, websites, etc.) that you can refer to to help me understand chronic kidney disease better?
- What are some resources for finding the best kidney disease friendly recipes?
That may seem like a lot of questions, but they are just a start to understanding your illness and what to do about it. Chronic kidney disease can be greatly impacted by the foods you eat, so maintaining the right diet can make all the difference when it comes to your life and well-being.
Remember, personalized treatment is key when dealing with chronic kidney disease. Be sure to discuss any concerns or questions you have with both your nephrologist and renal dietitian. With their guidance, you can make dietary changes that will improve your overall health and potentially slow the progression of CKD (CKD grocery list).
Understanding the 5 Stages of CKD
It's crucial to know the stage of chronic kidney disease you're in to take appropriate steps for your health and well-being. The five stages of CKD are determined by a patient's glomerular filtration rate (GFR) and proteinuria, which is the amount of protein in urine. Understanding these stages helps patients with CKD progression, treatment options, and lifestyle changes.
Here are three items that can help you understand the importance of knowing your CKD stage:
- Each stage has different treatment options, so knowing where you stand can help determine what therapies or medications may be necessary.
- Monitoring health is essential as it allows doctors to track whether there is any decline in kidney function or if complications arise.
- Early detection and intervention can slow down or halt CKD progression, but this requires awareness of one's current stage.
A normal eGFR is 60 or higher, while an eGFR less than 60 for three months or more may indicate kidney problems and increase the risk of CKD progression to kidney failure.
To better understand the different stages of CKD based on eGFR levels, here is a table that shows how they are classified:
| Stage | Description |
| 1 | Kidney damage with normal or high GFR (eGFR >90) |
| 2 | Mild decrease in GFR (eGFR = 60-89) |
| 3a | Moderate decrease in GFR (eGFR = 45-59) |
| 3b | Moderate decrease in GFR (eGFR =30-44) |
| 4 | Severe decrease in GFR (eGFR =15-29) |
| 5 | Kidney failure (eGFR <15) aka End Stage Kidney Disease |
It's important to note that some people may not experience symptoms until later stages of CKD when significant damage has been done. Therefore, regular monitoring with blood tests and urine samples is critical for those at risk or already diagnosed with kidney disease. Taking appropriate steps early on can improve outcomes and quality of life for those living with chronic kidney disease (How Quickly Will My Chronic Kidney Disease Progress To Dialysis).

Personalized Treatment and Care Planning
Take control of your kidney disease and improve your quality of life by working with healthcare professionals to create a personalized treatment plan that meets your unique needs. Collaborative planning is key to ensuring that you receive the best possible care.
Your nephrologist will work with you to develop a personalized medical plan that takes into account your stage of CKD, other health conditions, and lifestyle factors. Care coordination is an essential aspect of managing chronic kidney disease. Be sure to communicate openly with your healthcare team about any concerns or questions you may have.
Shared decision making involves discussing treatment options and weighing the benefits and risks together with your doctor. This process helps ensure that you are receiving treatments that align with your goals and values. Patient engagement is crucial in achieving optimal outcomes for individuals living with chronic kidney disease.
By taking an active role in the management of your condition, you can better understand how to manage symptoms, monitor changes in kidney function, and make informed decisions about treatment options. Remember to stay engaged throughout the course of treatment as this will help ensure success in managing chronic kidney disease over time.
Potential Treatment Options
The treatment options for chronic kidney disease aim to slow the progression of the disease, manage symptoms, and minimize complications. The choice of treatment depends on the stage of CKD and the underlying cause.
In the early stages, lifestyle modifications such as adopting a healthy diet low in salt and protein, managing blood pressure and blood sugar levels, and maintaining a healthy weight can be effective. Medications may be prescribed to control hypertension, reduce proteinuria, and manage complications like anemia and bone disease.
As CKD progresses, medical interventions such as dialysis or kidney transplantation may be necessary. Dialysis involves the use of a machine to filter waste and excess fluids from the blood, either through hemodialysis or peritoneal dialysis.
Kidney transplantation is considered the optimal treatment option, providing a long-term solution to restore kidney function. However, it may require immunosuppressive medications to prevent organ rejection.
Other supportive measures include managing cardiovascular risk factors (ckd and heart disease), such as cholesterol and lipid control, and addressing nutritional deficiencies. Regular monitoring and close collaboration with healthcare providers are essential to tailor treatment plans to individual needs and ensure optimal management of CKD.
It is important for individuals with CKD to work closely with their healthcare team to determine the most appropriate treatment approach based on their specific condition, stage of CKD, and overall health status.
Importance of Education and Involvement
You can enhance your understanding of chronic kidney disease and improve your health outcomes by actively educating yourself and getting involved in your care plan. Education is an essential component of managing chronic kidney disease effectively.
By learning about the condition, its causes, symptoms, and treatment options, you can make informed decisions about your health and take actions to manage the condition better. A knowledgeable patient is more likely to adhere to their treatment plan, make healthier lifestyle choices, and experience better health outcomes.
Involvement in your care plan is equally important. By collaborating with your healthcare team, you can become an active participant in developing a personalized treatment plan that meets your unique needs.
This approach allows you to have a say in the type of care you receive and empowers you to take ownership of your health. Involvement also means taking responsibility for making necessary lifestyle changes such as dietary modifications or exercise routines that will help slow down the progression of the disease.
The benefits of education and involvement are numerous. You will feel more confident and empowered in taking charge of your health when you understand chronic kidney disease better. You will also be able to communicate more effectively with your healthcare team regarding concerns or questions that may arise during treatment.
With knowledge comes power, power over a chronic illness like CKD that may seem overwhelming at first but can be managed successfully with the right education, involvement, support from family members and friends alongside medical professionals who are committed to seeing patients thrive even after diagnosis.
| Factor | Impact |
| Increased Knowledge | Better Health Outcomes |
| Empowered Patient | Collaborative Care |
| Improved Communication | Enhanced Quality Of Life |
The above table highlights some emotional responses associated with being educated about CKD while being involved with one's doctor's care plan; it all culminates into improved quality of life overall as one gains increased knowledge on CKD and its management.
Your Nephrologist Is Your Best Resource If You Have CKD
You've now learned the importance of asking your nephrologist the right questions when it comes to managing your chronic kidney disease.
From understanding the symptoms and causes of CKD to personalized treatment options, this article has provided you with a comprehensive guide to help you take control of your health (Comprehensive Healthy Renal Diet Grocery List Guide).
Remember that early detection and intervention can make a significant impact on living a fulfilling life with CKD. By asking your nephrologist about dietary goals, potential treatments, and involvement in your care planning, you're taking an active role in managing your condition.
Stay informed and educated about the stages of CKD and available treatment options so that you can work together with your healthcare team towards achieving optimal kidney health.