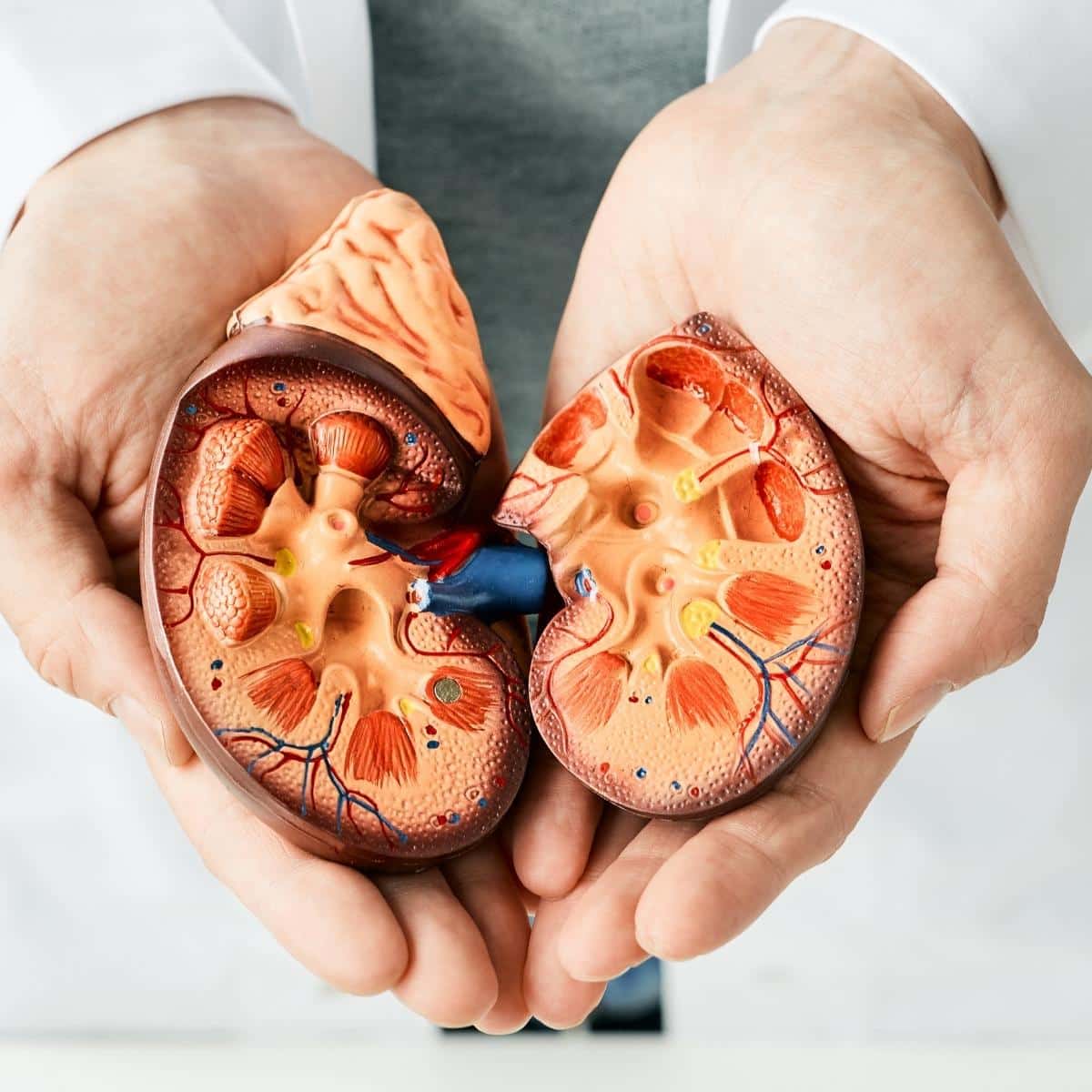
How Quickly Will My Chronic Kidney Disease Progress To Dialysis
Are you worried about how quickly your chronic kidney disease (CKD) will progress to dialysis? It's a valid concern, but the progression of CKD can actually vary greatly from person to person.
Your lifestyle, genetics, and other factors all play a role in how fast your renal function declines. In this article, we'll explore the different stages of kidney disease, the indicators and predictors of progression, and lifestyle changes that can help slow down decline (food for your stage of chronic kidney disease).
By understanding more about how your CKD may progress and taking steps to manage it proactively, you can feel more confident in your ability to serve others while living with this condition (chronic kidney disease diet food list).
Jump to:
- What Are The Stages of CKD?
- Factors Affecting Progression
- Indicators of Progression
- Difficulties in Prediction
- Lifestyle Changes
- Follow The Correct Meal Plan To Stop The Progression Of Kidney Disease
- Medication and Discontinuation
- Risk Factors for Rapid Decline
- Predictors of Fast CKD Progression
- Managing Accelerated Decline in Kidney Function
- FAQs for Chronic Kidney Disease
- Lifestyles Changes Can Slow Down Your Chronic Kidney Disease Progress To Dialysis
What Are The Stages of CKD?
As you go through the stages of chronic kidney disease (CKD), it's important to understand the changes happening in your body and how they can affect your overall health.
There are five stages of CKD, with stage one being the mildest and stage five being end-stage renal disease (ESRD). In the earlier stages, you may not experience any symptoms, but as your kidneys continue to decline in function, symptoms may arise, such as fatigue, swelling in the legs or feet, dry skin, and itching.
In stages one and two of CKD, there's a mild loss of kidney function and some signs of kidney damage. While you may still not experience any noticeable symptoms of kidney disease during this stage, it's important to make lifestyle changes such as eating a healthy diet low in sodium to slow down CKD progression.
Stage three is when kidney function drops significantly and patients may begin experiencing symptoms such as high blood pressure or anemia.
Stage four is when kidney function has declined severely and dialysis or a kidney transplant may be necessary soon. It's essential to work closely with your healthcare team during this time to manage complications and prepare for treatment options.
Understanding these stages can help you take charge of your health by making informed decisions about lifestyle modifications that can help slow down progression towards dialysis.
For More Recipes and Ideas --->> Get Your Free Meals and Recipes That Are Perfect for Pre-Dialysis Diets, Pre-Dialysis with Diabetes, or Dialysis Diets.
Factors Affecting Progression
Understanding the factors that impact the advancement of kidney disease can be crucial for those worried about its potential effects. There are several factors that can affect how quickly your chronic kidney disease progresses to dialysis.
These may include underlying health conditions, such as high blood pressure or diabetes, which can worsen kidney function over time. Additionally, certain lifestyle choices and habits, such as smoking or not following a proper diet, can also contribute to a faster progression of the disease.
Other factors that play a role in the progression of CKD include age and genetics. As you get older, your kidneys naturally begin to lose function, making it more difficult for them to filter waste products from your blood properly. Similarly, if you have a family history of kidney disease or other related conditions, you may be at higher risk for developing CKD yourself.
It is essential to keep these factors in mind when monitoring your kidney function and working with your healthcare provider to manage any underlying conditions.
While there is no way to predict exactly how quickly your chronic kidney disease will progress towards dialysis, understanding the various factors that impact its advancement can help you take steps towards managing the disease effectively.
By staying on top of any underlying health concerns and making positive lifestyle changes where necessary, you may be able to slow down or even halt the progression of CKD altogether.
Remember that early detection and treatment are key when it comes to managing this condition successfully.
Indicators of Progression
To effectively monitor the progression of your kidney disease, it's important to be aware of the various indicators that can signal a decline in kidney function.
One key indicator is a decrease in your estimated glomerular filtration rate (eGFR), which measures how well your kidneys are filtering waste from your blood. A drop in eGFR may suggest that your condition is worsening and may indicate the need for closer monitoring or more aggressive treatment.
Another indicator of progression is an increase in proteinuria, which means there's an abnormal large amount of protein in your urine. This can be a sign that your kidney damage has increased and that you're at higher risk of heart disease, stroke, and other complications. Your kidney doctor may recommend additional tests or medication to help manage this symptom and slow down further damage.
Finally, high blood pressure can also be an indicator of worsening kidney function. Over time, high blood pressure can cause damage to the tiny blood vessels in the kidneys, leading to decreased function and eventually dialysis or transplant. It's important to work with your healthcare team to manage hypertension through lifestyle changes and medication if necessary, as this can significantly slow down the progression of chronic kidney disease (reduce sodium intake on a renal diet).
Difficulties in Prediction
Predicting the future of your kidney health can be a real headache, with no surefire way to tell what might happen next. While there are some indicators that doctors can use to estimate how quickly your CKD will progress to dialysis, these predictions aren't always accurate.
One difficulty is that every patient's experience with CKD is unique. Even if two people have the same stage of CKD and similar medical histories, their rates of progression may differ. This means it's difficult to create one-size-fits-all guidelines for predicting CKD progression.
One of the reasons why it’s difficult to predict how quickly CKD will progress is that multiple factors can influence the speed of progression. Some of these factors include the following:
Overall Health: Your overall physical and mental wellness will play a role in how quickly your kidney function declines.
Medications: Certain medications like ACE inhibitors or ARBs can slow down the rate at which kidneys deteriorate, while others can cause further damage to the kidneys.
Blood Pressure: High blood pressure puts extra strain on kidneys leading them towards damage.
Blood Sugar Levels: Poorly controlled diabetes accelerates the rate of kidney damage.
Proteinuria: Increased amounts of protein in urine indicate increased kidney damage.
Additionally, factors such as age, sex, race, and other health conditions can all affect how rapidly CKD progresses.
Another challenge in predicting CKD progression is that symptoms don't always match up with the severity of the disease. For example, someone with advanced-stage CKD may not have any noticeable symptoms at all. On the other hand, someone with early-stage CKD may experience swelling or other symptoms that suggest more advanced disease than they actually have.
Finally, it's worth noting that while dialysis is often seen as the ultimate endpoint for those with severe CKD, it's not always necessary or appropriate for everyone. Depending on your overall health and goals of care, you may be able to manage your kidney disease without ever needing dialysis. So even if your doctor predicts rapid progression to end-stage renal disease (ESRD), there is still hope for managing your condition effectively without undergoing dialysis treatment.
In summary, predicting how quickly your CKD will progress to dialysis can be challenging due to the unique nature of every patient's experience with the disease. Symptoms may not always match up with severity, and factors such as age, sex, race, and other health conditions can all affect the progression rate (progression of symptoms for CKD).
However, by working closely with your doctor and paying attention to indicators such as overall health, medication use, systolic blood pressure, and sugar levels, you can take steps towards slowing down or even stopping its progression. Remember that while dialysis is often seen as a last resort for those with severe CKD, it may not be necessary or appropriate for everyone.
Lifestyle Changes
If you want to take control of your kidney health, making lifestyle changes can be a great place to start. It's important to remember that CKD progresses slowly over time, and making positive lifestyle changes can help slow down its progression. A healthy diet rich in fruits, vegetables, and lean meats can improve blood pressure and maintain kidney function.
Another important lifestyle change to consider is regular physical activity. Exercise promotes overall health by maintaining a healthy weight, reducing stress levels, and lowering your risk of cardiovascular disease. However, it's important to consult with your healthcare provider before starting any new exercise regimen or if you have other medical conditions that may affect your ability to exercise.
Finally, quitting smoking and limiting alcohol consumption are also crucial steps in managing CKD. Both smoking and excessive alcohol intake can worsen kidney function by increasing blood pressure and damaging blood vessels in the kidneys.
Taking small steps towards a healthier lifestyle can make a big difference in slowing down the progression of CKD and improving overall health outcomes.

Follow The Correct Meal Plan To Stop The Progression Of Kidney Disease
Dialysis can be a very scary endpoint to look forward to and I completely understand your desire to prevent placement on dialysis. Regardless of how much protein you have in your urine or what stage of kidney disease you are in, as long as it's pre-dialysis, you can slow the progression through the implementation of a healthy diet.
If you're in stages one or two of pre-dialysis kidney disease, you should work hard to control your blood pressure, diabetes, and any sort of heart disease that you have. If you need meal plans to help you prepare nutritious yet delicious meals, you can check out our meal planning program for Free 7 Day Meal Plan. Stage 1 kidney disease diet is really just eating more fruits and vegetables as well as less sodium and managing your weight.
If you've progressed to stages three or four of pre-dialysis kidney disease, you should look into our meal plans that we have on the renaldiethq.com website to help you manage the low-protein and diabetes meal plan that you need to also have nutritious and delicious meals.
Your stage is often affected by many things and you can be in chronic kidney disease stage IIIB which is a little higher priority and a little stricter than the diet for CKD Stage 1.
Stage III kidney failure means you really need to start working to control protein and sodium in your diet in addition to making it a priority to maintain excellent blood pressure control.
Medication and Discontinuation
In addition to following a kidney-friendly diet, you can also manage your kidney health with medication and by discussing options for discontinuing medications that may harm your kidneys.
Medications are commonly used to treat the complications associated with CKD, such as high blood pressure, anemia, and bone disease. Taking these medications as prescribed can help slow down the progression of CKD, which may delay the need for dialysis or a kidney transplant.
However, it's important to note that some medications can actually harm your kidneys and worsen CKD. That's why you should discuss all of your medications with your healthcare provider, including over-the-counter drugs and supplements.
Your provider may recommend changing or stopping certain medications to prevent further damage to your kidneys. It's crucial to follow their recommendations carefully.
To effectively manage your kidney health through medication, here are three tips:
- Take all prescribed medications exactly as directed by your healthcare provider.
- Discuss all of your current medications with your provider to identify any that might be harmful to your kidneys.
- Be aware of potential side effects and report any new symptoms or changes in how you feel to your healthcare provider immediately.
Remember that managing CKD requires a comprehensive approach that includes lifestyle changes, regular medical care, and taking prescribed medication. By being proactive about managing both the benefits and risks of medication use in CKD, you can take control of this aspect of your health journey and make progress towards preserving kidney function for as long as possible.
Risk Factors for Rapid Decline
Managing your kidney health with medication is vital, but it's also important to be aware of the risk factors for rapid decline.
Chronic kidney disease can progress quickly in some individuals, leading to a higher likelihood of needing dialysis. Some of the factors that contribute to this include age, genetics, and underlying medical conditions such as high blood pressure or diabetes.
Age is a significant factor when it comes to the progression of chronic kidney disease. As we age, so do our kidneys. Typically, people above the age of 60 are more likely than not to develop CKD.
Additionally, genetics play an important role in determining how quickly your kidneys will deteriorate over time. If you have a family history of chronic kidney disease (can kidneys repair themselves) or other related conditions such as polycystic kidney disease, it's essential to monitor your kidney function regularly.
Underlying medical conditions like high blood pressure and diabetes can also increase your risk for rapid decline in kidney function. It's critical to manage these conditions carefully by taking medications as prescribed by your doctor and making lifestyle changes like adopting a healthy diet and exercising regularly. By doing so, you may be able to slow down the progression of chronic kidney disease and avoid dialysis altogether.
In conclusion, understanding the risk factors for rapid decline in chronic kidney disease is crucial for managing your overall health effectively. Age, genetics, and underlying medical conditions all play a role in determining how quickly your kidneys will deteriorate over time (ckd and diabetes medications).
By staying informed about these factors and taking care of yourself through proper management techniques like medication adherence and lifestyle changes, you may be able to slow down or even prevent further damage from occurring.
Predictors of Fast CKD Progression
Knowing the predictors of fast CKD progression can help you take proactive steps to protect your kidney health. Firstly, high blood pressure is a significant predictor of rapid decline in kidney function. Therefore, it's essential to keep your blood pressure under control with medication and lifestyle changes such as exercise and a healthy diet (high blood pressure and kidney disease).
Secondly, proteinuria or the presence of excess protein in urine is also a strong indicator of fast CKD progression. Some studies also suggest that the presence of protein in urine accelerates kidney damage by increasing inflammation and scarring in the kidneys. You can reduce proteinuria by limiting your intake of animal proteins, especially red meat, and taking medication prescribed by your doctor.
Lastly, smoking has been found to be a crucial factor in accelerating CKD progression. It increases oxidative stress on the kidneys and causes inflammation that damages them further. Quitting smoking can significantly slow down the rate of decline in kidney function and improve overall health outcomes.
By knowing these predictors, you can take action towards preserving your kidney function for longer periods before dialysis becomes necessary. Make sure to consult with your doctor regularly about any changes in kidney function or other risk factors that may affect its health. With proper care and management, you have the power to make a positive impact on your overall well-being.
Managing Accelerated Decline in Kidney Function
If your kidney function is declining more rapidly than expected, it's important to work with your healthcare team to identify potential causes and develop a treatment plan (kidney disease treatment diet).
They will likely perform a series of tests to determine the underlying cause and assess the extent of kidney damage. These tests may include blood tests, urine tests, imaging studies, and possibly a kidney biopsy.
Once the cause is identified, your healthcare team will develop a personalized treatment plan. This plan may involve lifestyle modifications, such as adopting a healthy diet low in salt and saturated fats, exercising regularly, and quitting smoking. Medications may also be prescribed to control blood pressure, manage diabetes, or treat any underlying conditions contributing to kidney damage (commonly prescribed medications for CKD).
In some cases, more aggressive interventions may be necessary. For example, if a blockage or narrowing of the blood vessels in the kidneys is causing the accelerated decline, a procedure called angioplasty may be performed to open up the blocked vessels. In severe cases, dialysis or a kidney transplant may be required.
It's important to remember that everyone's experience with chronic kidney disease is unique. While some people may progress quickly towards dialysis or transplantation, others may have a slower decline in kidney function.
By working with your healthcare team and following a kidney-friendly diet plan, you can help improve the health of your kidneys and potentially slow down their decline over time.
FAQs for Chronic Kidney Disease
If you're curious about how race and ethnicity can impact the progression of chronic kidney disease (CKD), there's evidence to suggest that certain populations may be more at risk for developing end-stage kidney disease.
Studies have shown that individuals who identify as Black, Hispanic, or Native American may be up to three times more likely to develop end-stage renal disease compared to those who identify as White. This may be due in part to disparities in access to healthcare, socioeconomic factors, and genetic predispositions (how to prevent end stage renal disease).
However, it's important to note that every person's experience with CKD is unique, and it's crucial to work closely with your healthcare team to monitor your individual progression and make informed treatment decisions.
Stress and mental health can indeed impact the progression of chronic kidney disease (CKD). Studies have shown that people with kidney disease experience high levels of stress and anxiety, which can worsen their condition (how to reduce stress naturally).
Stress activates the sympathetic nervous system, leading to increased blood pressure, which in turn damages the kidneys. Additionally, depression has been linked to an increased risk of CKD progression and mortality.
Therefore, it's crucial for individuals with CKD to manage their stress levels and seek help if experiencing symptoms of depression or anxiety. Some effective strategies include exercise, meditation, therapy, and support groups.
By prioritizing your mental health alongside medical treatment, you may be able to slow progression of your CKD.
You might think of exercise as an investment in your health, and it turns out that this investment can pay off for those with chronic kidney disease (CKD).
Research shows that regular physical activity can help slow down the progression of CKD. Exercise helps your kidneys function better. It also lowers blood pressure and reduces inflammation throughout the body, both of which are important factors in slowing CKD progression.
So, if you're looking for a way to take control of your health and potentially improve your kidney function, adding exercise to your routine could be a good place to start (exercise for CKD Patients).
If you're looking for alternative treatments or therapies that can slow or reverse the progression of chronic kidney disease (CKD), there are several options available.
One approach is to focus on managing underlying health conditions that may contribute to CKD, such as high blood pressure and diabetes. This may involve lifestyle changes like modification of diet and exercise, as well as medication management.
Additionally, some studies suggest that certain supplements and herbs, such as omega-3 fatty acids and Chinese herbal medicine, may have a beneficial effect on kidney function. It's important to speak with your healthcare provider about these potential treatments and determine the best course of action for your individual needs (ckd progression).
Did you know that age is a significant factor in the progression of chronic kidney disease (CKD)? According to recent studies, patients over the age of 65 have a higher likelihood of developing end-stage renal disease (ESRD) and requiring dialysis.
In fact, adults over the age of 65 account for more than one third of all CKD cases in the United States. While there are undoubtedly other factors at play in CKD progression, including underlying health conditions and lifestyle factors, your age can play a critical role in determining your risk level.
If you're concerned about the potential need for dialysis as your CKD progresses, it's essential to talk with your doctor about proactive steps you can take to protect your kidney function and manage any underlying conditions that may be contributing to the problem.
Lifestyles Changes Can Slow Down Your Chronic Kidney Disease Progress To Dialysis
You now have a better understanding of the factors that affect the progression of your chronic kidney disease (CKD) and how to slow it down. While there's no guaranteed timeline for when you'll need dialysis, taking steps to control your blood pressure and diabetes, maintaining a healthy kidney-friendly diet plan, and avoiding harmful substances can make a significant difference in slowing the decline of your kidney function (improving kidney function with diet).
Some may argue that making these lifestyle changes can be difficult or burdensome. However, it's important to remember that even small changes can have a big impact on your health.
Seeking support from healthcare professionals, family members, or friends can also help you stay motivated and accountable towards achieving better health outcomes. Remember that you're not alone on this journey. With proper self-care and medical attention, you can take charge of your CKD and live a healthier life (




















This is a very helpful article. I didn't know that there is a greater risk of mortality for CKD patients if they have diabetes until I saw your article. My sister was diagnosed with diabetes prior to getting diagnosed with CKD. Now I know that we should pay more attention to her health. I'll be sure to pass the information along to my parents and see what we can do about it. Thanks a lot!
Thanks for the info, I have advanced cirrhosis and by luck my hand doctor had blood work done and report said kidney failure, I am a little nervous