Colon And Kidney Disease
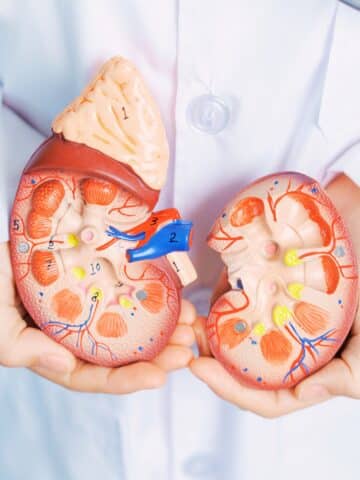
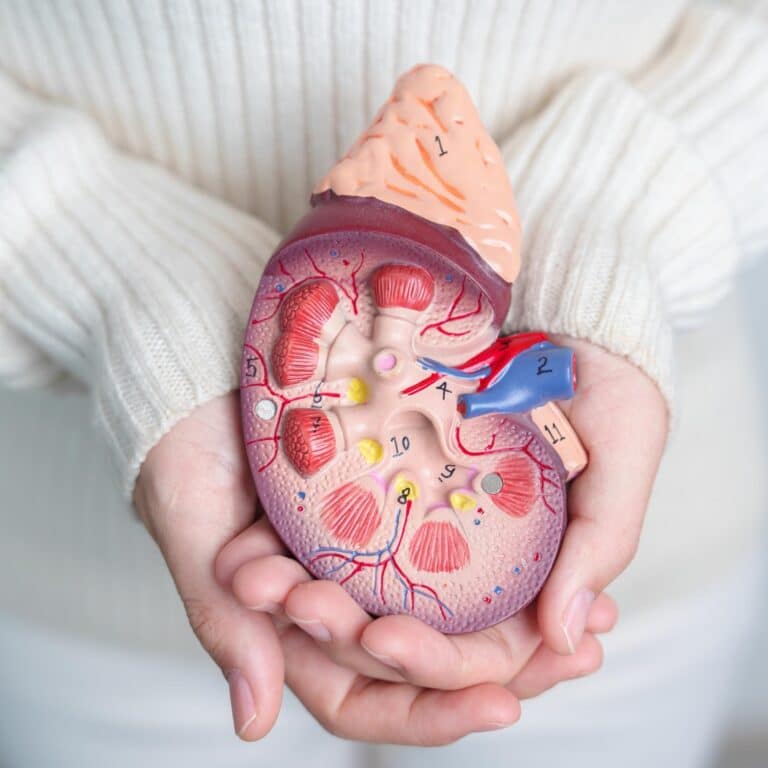
Are you aware of the connection between your colon and kidney health?
Chronic kidney disease is a common comorbidity of colorectal cancer. Moreover, individuals who undergo a kidney transplant are at higher risk for colon cancer. Diabetes, another common cause of CKD, also increases the risk of colorectal cancer.
Colorectal cancer is the second leading cause of mortality in patients with cancer in the United States. Every year, over 50,000 people die from this medical condition, and about 140,000 more cases are diagnosed.
Age plays a large part in colorectal cancer. 90% of patients with colorectal cancer are over the age of 50. Symptoms that may determine you have the cancer include bloody stool, stomach pain or cramps that will not go away, and weight loss with no known cause (kidney disease weight loss).
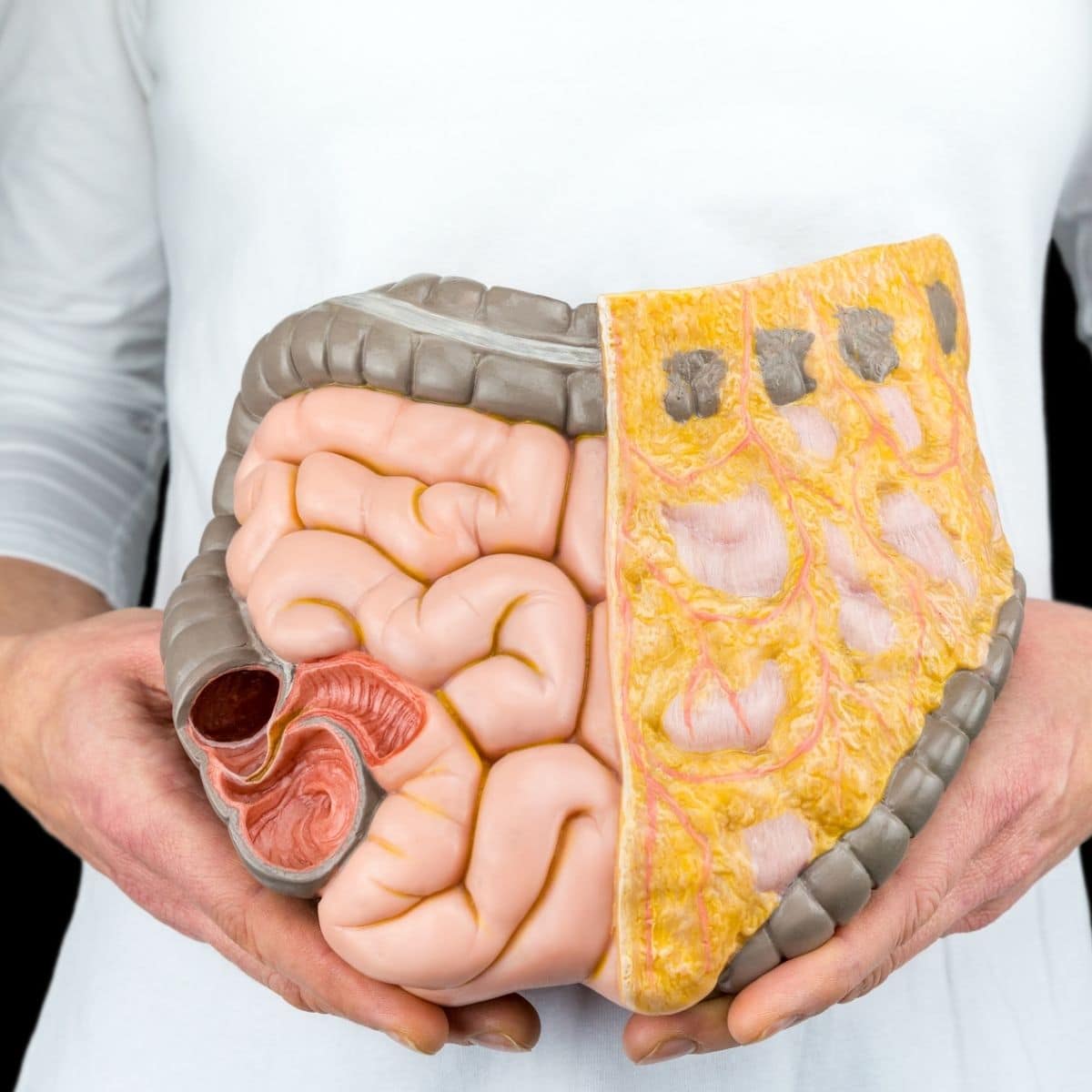
Knowing the symptoms of colorectal cancer is vital. Aside from symptom monitoring, various screening methods such as colonoscopies are available.
In the context of CKD, it is crucial to understand the impact of uremic toxins. These toxins, generated from microbial fermentation, are protein-bound solutes derived from precursor substances.
Can diet improve ckd symptoms? Imbalances in intestinal microbiota, favoring proteolytic microorganisms and leading to increased toxin precursor production through fermentation in uremia, play a significant role. By familiarizing yourself with the risks, symptoms, and screenings associated with colon health and CKD, you can make informed decisions about your well-being.
In this article, we will look at various factors and associations that link chronic kidney disease with colorectal cancer, as well as what you can do in terms of early prevention and prompt treatment of this condition.
Jump to:
- Key Takeaways
- What Is Colon Cancer?
- Intestinal Microbiota and CKD
- Uremic Toxins and CKD
- Colorectal Cancer and CKD
- Screening Risks for CKD Patients
- Symptoms of Colorectal Cancer
- Preventing Colon Cancer
- Shift in Intestinal Microbiota
- Therapeutic Interventions for CKD
- Diagnosis and Treatment of Colon Cancer
- Impact of Diet on CKD and Colon Cancer
- FAQs About Colon And Kidney Disease
- Kidney Health and Gut Health Go Hand In Hand
Key Takeaways
- Colon cancer risk is higher in CKD populations, especially in those who have had a kidney transplant, and diabetes increases the risk of colorectal cancer which is one of the leading causes of CKD.
- Symptoms of colorectal cancer include bloody stool, stomach pain or cramps that will not go away, and unexplained weight loss. Maintaining a healthy weight, eating a well-balanced diet, being physically active, avoiding smoking, and heavily moderating alcohol consumption can reduce your risk of colon cancer.
- There are many screenings for colon cancer, including colonoscopy, but there are risks for CKD patients, especially with bowel cleansing products containing sodium phosphate. Always ensure your doctor knows about your status of renal impairment prior to having a colonoscopy.
- Uremic toxins, which are essentially protein-bound solutes, are generated metabolically from precursors originating from microbial fermentation, and the balance of intestinal microbiota is shifted in favor of proteolytic microorganisms producing more toxin precursor by fermentation in uremia.
For More Recipes and Ideas --->> Get Your Free Meals and Recipes That Are Perfect for Pre-Dialysis Diets, Pre-Dialysis with Diabetes, or Dialysis Diets.
What Is Colon Cancer?
Colon cancer, also known as colorectal cancer, is a type of cancer that affects the colon or rectum, which are both part of the large intestine within the gastrointestinal tract. It typically begins as a growth called a polyp on the inner lining of the intestinal wall. Over time, these polyps can become cancerous and develop into tumors.
Colon cancer is one of the most common types of cancer worldwide and can affect people of all ages, although the risk increases with age. The exact cause of colon cancer is not fully understood, but certain factors such as family history, genetic mutations, inflammatory bowel disease, unhealthy lifestyle habits, and certain inherited conditions can increase the risk.
Symptoms of colon cancer may include changes in bowel habits, persistent abdominal discomfort, blood in the stool, unexplained weight loss, and fatigue. Early detection through regular screenings, such as colonoscopies, is crucial for timely diagnosis and effective treatment.
Treatment options for colon cancer may include surgery, radiation therapy, chemotherapy, targeted therapies, and immunotherapy, depending on the stage and extent of the disease.
Intestinal Microbiota and CKD
If you have CKD, it's important to understand the microbial imbalance that occurs in your intestinal microbiota as this can have effects on your gut health. This shift favors proteolytic microorganisms, which produce more toxin precursors by fermentation. As a result, there is an increased generation and concentration of uremic toxins, which can eventually lead to renal failure.
Moreover, this gut dysbiosis causes abnormal intestinal motility, intestinal barrier function or intestinal permeability, and prolongs colon transit in uremia. This increases the generation of bacterial toxins and time for their absorption within the intestinal environment. The bacterial species prone to generate uremic toxins are privileged in uremia and outnumber protective species such as Lactobacilli.
Fortunately, probiotic therapy has been shown to provide specific benefits by creating a more favorable balance in the composition of intestinal microbiota. Additionally, metabolic endotoxemia can be prevented or treated through dietary intervention aimed at reducing fat intake or increasing dietary fibre intake.
These therapeutic interventions offer hope for those with CKD who wish to improve their condition and avoid further complications associated with their disease.
Uremic Toxins and CKD
You need to be aware that the balance of your intestinal microbiota can impact the production of uremic toxins, which can have negative effects on your health. Chronic conditions linked to changes in the gut microbiome are also associated with renal failure.
Uremic toxins, those harmful substances that accumulate in your body due to chronic kidney disease, play a significant role in your overall health. These toxins, which are essentially waste products generated from the breakdown of proteins, can have detrimental effects on various organs and systems.
As a person living with CKD, it's crucial for you to understand the impact of uremic toxins and take proactive steps to manage their levels.
Renal impairment in adults with kidney disease leads to a buildup of these toxins in your bloodstream, as your kidneys are unable to effectively filter them out. This accumulation can result in a range of complications, including cardiovascular problems, bone disease, anemia, and inflammation.
Uremic toxins can also adversely affect your immune system, further compromising your body's ability to fight infections.
To mitigate the harmful effects of uremic toxins, it is essential to work closely with your healthcare team. They can provide guidance on various treatment options, such as dialysis or kidney transplantation, to help remove these toxins from your body.
Additionally, following a kidney-friendly diet, which limits the intake of protein and certain minerals, can help reduce the production and accumulation of uremic toxins.
Regular monitoring of renal dysfunction and serum concentrations of uremic toxins through blood tests is crucial to gauge the effectiveness of your treatment and make necessary adjustments.
By staying informed and actively engaging in your care, you can take control of managing uremic toxins and work towards preserving your overall well-being while living with CKD.
Colorectal Cancer and CKD
Colorectal cancer and chronic kidney disease share a significant association (link between constipation and CKD)that you should be aware of as an individual living with CKD. Although the exact mechanisms are still being studied, researchers have identified several factors that contribute to this link.
Individuals with CKD, especially those who have undergone kidney transplantation, face a higher risk of developing colorectal cancer compared to the general population. The reasons behind this association are multifaceted and complex.
One potential factor is the compromised immune system associated with CKD. As your renal function declines, your immune system may weaken, making it more challenging for your body to defend against the growth and spread of tumor cells. Additionally, chronic inflammation, which is often present in CKD, may play a role in the development of colorectal cancer.
Moreover, the presence of diabetes, a leading cause of CKD, further increases the risk of colorectal cancer. Diabetes disrupts the body's ability to regulate blood sugar levels, resulting in harmful changes in the epithelial cells lining the colon and rectum. When diabetes and CKD coexist, the risk of developing colorectal cancer becomes even more pronounced.
While the precise mechanisms behind the association between colorectal cancer and CKD are not fully understood, it is evident that CKD, particularly when combined with factors like compromised immunity and the presence of diabetes, heightens the risk of developing colorectal cancer.
This underscores the importance of comprehensive healthcare management for individuals with CKD. Regular monitoring, ongoing communication with your healthcare provider, and adherence to your treatment plan are essential (kidney disease treatment diet).
Screening Risks for CKD Patients
Watch out for the risks of screening for colorectal cancer as a CKD patient, as some bowel cleansing products can be harmful to your kidneys and cause kidney failure. It's crucial to inform your doctor about your kidney function and have your glomerular filtration rate checked before undergoing any colonoscopy.
Screening is vital for early detection of colorectal cancer, especially in patients with diabetes who have a higher risk of developing this type of cancer. Colon cancer is one of the leading causes of CKD and has higher incidence rates in post-kidney transplant patients.
Colonoscopies are considered the gold standard in detecting colon cancer, but they carry certain risks for CKD patients. Bowel-cleansing products that contain sodium phosphate (OSP) can cause acute phosphate nephropathy and lead to kidney failure in some individuals.
The FDA warns against using OSPs as laxatives or before colonoscopies due to their potential harm to people with kidney disease. Always discuss these risks with your healthcare provider before undergoing any procedure.
Early detection through regular screenings like colonoscopy is crucial in preventing colorectal cancer. However, it's essential to balance its benefits with potential risks. Work closely with your healthcare team when deciding on the best screening option for you and manage any medical concerns that could affect the procedure's outcomes effectively.
Symptoms of Colorectal Cancer
When it comes to colon cancer, it is crucial to be aware of the symptoms that may indicate its presence. Recognizing these signs early on can lead to timely medical intervention and improved outcomes. While these symptoms (signs and symptoms of kidney failure) are not exclusive to colon cancer and can be caused by other conditions, being mindful of them can help you make informed decisions about your health.
One potential symptom of colon cancer is a change in bowel habits. You may notice persistent changes in your regular bowel movements, such as diarrhea or constipation in patients that lasts for an extended period. Additionally, you might experience a feeling of incomplete bowel emptying after a bowel movement.
Another symptom to be mindful of is rectal bleeding. This may manifest as bright red blood in your stool or blood present on the toilet paper after wiping. It is important to note that not all cases of rectal bleeding are indicative of colon cancer, but it should be evaluated by a healthcare professional to determine the cause.
Unexplained and persistent abdominal discomfort or pain may also be a sign of colon cancer. This discomfort can range from cramps to persistent stomach aches that do not go away even with over-the-counter remedies.
Unexplained weight loss is another potential symptom to be aware of. If you are losing weight unintentionally without changes in your diet or physical activity, it could be a cause for concern.
Lastly, fatigue and weakness can also be symptoms of colon cancer. If you find yourself feeling excessively tired and lacking energy despite getting enough rest, it is essential to discuss this with your healthcare provider.
It is important to remember that experiencing these symptoms does not necessarily mean you have colon cancer, as they can be caused by other conditions. However, if you are experiencing any of these symptoms, it is crucial to consult with a healthcare professional for proper evaluation and diagnosis. Early detection and intervention can significantly improve the outcomes for colon cancer.
Preventing Colon Cancer
To reduce your risk of developing colon cancer, adopting a healthy lifestyle is key. Colon cancer prevention is very similar to what helps to reduce your chronic kidney disease. In order to reduce your risk of colon cancer, it is recommended that you:
- Maintain a healthy weight
- Eat a well-balanced diet
- Be physically active
- Avoid smoking
- Heavily moderate your alcohol consumption
Regular exercise and maintaining a healthy weight can help lower your risk of developing this deadly disease.
In addition, eating a balanced diet with plenty of fiber-rich fruits and vegetables can also help decrease your chances of developing colon cancer. Dietary factors have been shown to play a crucial role in the development of colon cancer.
Eating red meat and processed foods has been linked to an increased risk, while consuming more plant-based foods can help protect against it. Moderating alcohol consumption is also important as excessive drinking has been associated with an increased risk of colorectal cancer.
Early detection through regular screenings such as colonoscopy is crucial for catching any potential problems before they become more serious. It's important to discuss any concerns with your doctor and ensure that they are aware of any kidney issues you may have prior to undergoing any screening procedures.
By adopting these healthy habits and staying on top of screenings, you can take control over your health and reduce your risk of developing colon cancer.
Shift in Intestinal Microbiota
Adopting a plant-based diet and increasing fiber intake can shift the balance of intestinal microbiota, potentially reducing the generation and concentration of protein bound uremic toxins in individuals with chronic conditions linked to changes in gut bacteria.
Gut dysbiosis, or an imbalance in the composition of intestinal microbiota, is common in patients with chronic kidney disease due to increased microbial fermentation of protein precursors into toxic solutes. However, selective diets excluding sources of specific toxins may be an alternative approach for decreasing toxin generation.
Prebiotics are non-digestible compounds that improve the composition and/or function of intestinal microbiota. Arabinoxylan-oligosaccharides (AXOS), galacto-oligosaccharides, resistant starch, inulin and lactulose have been shown to decrease the generation and concentration of uremic toxins by decreasing fecal phenol and ammonia while also restoring insulin sensitivity and reducing insulin resistance in CKD animals.
In addition, gum Arabic supplements have been found to decrease urea concentration but not creatinine levels in non-dialysis CKD patients (cookbook for CKD patients) on a low-protein diet. Nonetheless, clinical studies on these therapies should be checked critically for evidence base.
Probiotics can provide specific benefits by creating a more favorable balance in the composition of intestinal microbiota. Lactic acid bacteria such as Lactobacilli and Bifidobacteria have been found to reduce urinary p-cresol levels in a placebo-controlled randomized trial conducted on subjects.
Lebenin has resulted in decreased plasma indoxyl sulphate levels while urease-expressing bacteria may decrease blood urea and markers related to kidney failure.
These interventions offer promising strategies for modifying gut dysbiosis-induced uremia; however, further randomized controlled trials are needed for conclusive recommendations regarding their use as therapeutic interventions for CKD patients experiencing shift effects within their intestinal microbiota.
Therapeutic Interventions for CKD
One promising approach for reducing the concentration of uremic toxins in individuals with chronic kidney disease is through the use of prebiotics and probiotics to modify gut dysbiosis-induced uremia.
Prebiotics are non-digestible compounds that improve the composition and function of intestinal microbiota, while probiotics create a more favorable balance in their composition.
Decreasing protein intake should also diminish the generation of uremic retention solutes. Veganism and vegetarian diets have been shown to decrease concentration and generation of protein-bound uremic solutes or their precursors. Selective diets excluding sources of specific toxins are an alternative.
Increasing dietary fiber intake has been found to decrease plasma-free indoxyl sulfate in hemodialysis patients with end-stage renal disease.
Resistant starch, inulin, lactulose, arabinoxylan-oligosaccharides (AXOS), galacto-oligosaccharides (GOS), and gum Arabic supplements have all been tested as potential interventions for individuals with CKD.
Resistant starch decreased plasma-free indoxyl sulfate, while AXOS decreased p-cresyl sulfate concentration while restoring insulin sensitivity in CKD animals.
GOS decreased cecal indoles and serum indoxyl sulfate levels, improved renal injury, stress markers, and apoptosis in ⅚ nephrectomized rats. Gum Arabic supplement decreases urea concentration but not creatinine in non-dialysis CKD patients on a low-protein diet. OF-IN impacts plasma concentration of p-cresyl sulfate but not indoxyl sulfate in maintenance hemodialysis patients with renal failure.

Diagnosis and Treatment of Colon Cancer
When it comes to the diagnosis and treatment of colon cancer, understanding the process and available options is essential for individuals like you.
If you suspect colon cancer or have been diagnosed with it, your healthcare team will guide you through the necessary steps to determine the extent of the disease and develop an appropriate treatment plan. Keep in mind that the information provided here is a general overview, and your healthcare provider will tailor the approach to your specific situation.
The diagnosis of colon cancer often begins with a thorough medical history review and physical examination. Your doctor may recommend additional tests, such as imaging studies like CT scans or MRIs, to evaluate the extent of the cancer and determine if it has spread to other parts of the body.
Additionally, a colonoscopy is commonly performed to visualize the colon and rectum, and tissue samples (biopsies) may be taken for further analysis.
For individuals with chronic kidney disease (CKD), special considerations are taken into account during the diagnosis and treatment of colon cancer. It is essential to inform your healthcare provider about your CKD status and any related treatments or medications.
This information will help them make appropriate decisions regarding diagnostic procedures and treatment options that are safe and suitable if you suffer from loss of kidney function. Once a diagnosis is confirmed, the therapeutic options for colon cancer typically involves surgery, chemotherapy, radiation therapy, or a combination of these modalities.
Surgery is often the primary treatment and involves removing the cancerous portion of the colon and nearby lymph nodes. In some cases, a colostomy or ileostomy may be necessary to redirect the bowel movements.
Chemotherapy may be recommended before or after colon cancer surgery to destroy any remaining cancer cells or reduce the size of the tumor. Radiation therapy, which uses high-energy X-rays or other types of radiation, may also be employed to target the cancer cells and shrink the tumor before surgery or alleviate symptoms in advanced cases.
Close monitoring of kidney function due to chronic kidney disease in patients undergoing therapy is crucial throughout the treatment process. Certain chemotherapy drugs and radiation therapies may cause renal dysfunction, and adjustments or alternative treatment options may be necessary to minimize the risk of further kidney damage.
During your treatment journey, open communication with your healthcare team is vital. They will provide you with detailed information about the potential side effects of treatment, manage any symptoms or complications, and offer support throughout the process.
Remember, each person's situation is unique, and your healthcare team will work with you to develop an individualized treatment plan that takes into account your overall health and CKD status. It is important to remain proactive in your healthcare, attend all scheduled appointments, and follow your healthcare provider's recommendations diligently.
By working closely with your medical team and maintaining a positive mindset, you can navigate the diagnosis and treatment of colon cancer with confidence and optimize your chances of successful outcomes.
Impact of Diet on CKD and Colon Cancer
Maintaining a healthy diet can significantly reduce your risk of developing certain types of cancer and chronic conditions. In particular, adopting a well-balanced diet can help prevent colon cancer and mitigate chronic kidney disease progression to end stage renal disease (dash diet for kidney disease).
Here are some ways in which you can modify your diet to reduce your independent risk factors:
- Increase fiber intake: Eating foods rich in fiber, such as fruits, vegetables, whole grains, and legumes, can promote bowel regularity and decrease the risk of colorectal cancer. Additionally, fiber may also improve kidney function in patients with CKD by reducing inflammation.
- Limit red meat consumption: Consuming large amounts of red meat has been linked to an increased risk of colon cancer. To reduce this risk factor, consider replacing red meat with plant-based protein sources or leaner meats like fish or poultry (low phosphorus meats).
- Reduce sodium and processed food intake: High sodium intake has been associated with an increased risk of CKD. Processed foods often contain high amounts of sodium, so it's important to read labels carefully and opt for fresh or minimally processed foods whenever possible.
In addition to dietary interventions, lifestyle modifications such as maintaining a healthy weight, exercising regularly, avoiding smoking, and moderating alcohol consumption can also help lower the risk for both colon cancer and CKD.
By incorporating these prevention strategies into your daily routine, you may be able to improve your overall health outcomes and reduce the likelihood of developing these chronic conditions.
FAQs About Colon And Kidney Disease
Dietary changes and probiotics have shown promise in improving the balance of intestinal microbiota and reducing the generation of uremic solutes in CKD patients.
By adopting a healthy and balanced diet that includes fiber-rich foods, CKD patients can promote the growth of beneficial bacteria in the gut and potentially reduce the production of harmful uremic solutes.
Additionally, probiotics, which are live microorganisms that confer health benefits, have been studied for their potential to modulate gut microbiota composition and function in CKD. Probiotic supplementation may help restore a more favorable microbial balance and decrease the production of uremic toxins.
However, it is important to note that the effects of dietary changes and probiotics can vary among individuals, and more research is needed to establish specific recommendations and evaluate their long-term impact on chronic kidney disease progression and related health outcomes.
As always, it is advisable for CKD patients to consult with their healthcare provider or a registered dietitian for personalized dietary guidance and recommendations tailored to their individual needs and condition.
To reduce your risk of developing colon cancer, CKD patients can take several preventative measures. One important step is to make dietary changes such as maintaining a healthy weight, eating a well-balanced diet, and being physically active.
Avoiding smoking and heavily moderating alcohol consumption can also help. Additionally, incorporating probiotics into your diet may improve the balance of intestinal microbiota and decrease the capacity to generate uremic solutes and their precursors in CKD patients.
Regular screenings for colon cancer are also essential. However, it's important to inform your doctor about your kidney function prior to having a colonoscopy as some bowel cleansing products containing sodium phosphate may be harmful to those with CKD.
By following these preventative measures, you can reduce your risk of developing colon cancer and promote overall health and well-being.
When undergoing colon cancer screenings, CKD patients face potential risks that should be carefully considered. Screening guidelines recommend a colonoscopy every 10 years, but CKD patients must inform their doctors about their kidney function before the procedure.
Bowel cleansing products containing sodium phosphate can cause acute phosphate nephropathy and kidney failure in some individuals, so alternative preparations may be necessary for CKD patients. Sedation options should also be discussed with your doctor, as some medications may not be safe for those with impaired kidney function (commonly prescribed medications for CKD).
Follow-up care is crucial to monitor any changes or complications after the screening. It is important to weigh the benefits of early detection against the potential risks, and to work closely with your healthcare team to ensure a safe and effective screening process.
While the clinical features of colorectal cancer can be similar for individuals with or without chronic kidney disease, CKD patients should be aware of certain potential complications.
CKD patients may experience a higher risk of developing colorectal cancer, and they should pay attention to any changes in their bowel habits, including blood in the stool, persistent stomach pain or cramps, unexplained weight loss, or changes in appetite.
However, it's important to note that these symptoms are not exclusive to CKD patients and can be indicative of various conditions. If you have CKD and experience any concerning symptoms, it is crucial to consult with your healthcare provider for further evaluation and appropriate management.
Early detection and timely intervention play a vital role in improving outcomes, and your healthcare team can guide you through the necessary steps for diagnosis and treatment.
Uremic toxins, the byproducts of protein metabolism that accumulate in the body due to impaired kidney function, significantly contribute to chronic kidney disease progression and related health complications. These toxins have various harmful effects on the body.
Uremic toxins promote inflammation, oxidative stress, and fibrosis within the kidneys, worsening renal function. They disrupt the delicate balance of gut microbiota, favoring the growth of harmful bacteria and leading to dysbiosis.
Systemically, uremic toxins have detrimental effects on multiple organs. They contribute to cardiovascular risks like atherosclerosis, coronary artery disease, hypertension, and left ventricular hypertrophy, increasing the risk of cardiovascular disease and cardiovascular mortality (exercise for healthy heart).
Uremic toxins also impact bone metabolism, leading to renal osteodystrophy and an elevated fracture risk. They impair immune function, making individuals with CKD more susceptible to infections. Additionally, these toxins have neurotoxic effects, contributing to cognitive impairment and peripheral neuropathy.
The accumulation of uremic toxins in CKD leads to progressive kidney function decline, exacerbates inflammation and fibrosis, and causes various systemic health issues. Managing uremic toxins through treatments such as dialysis or kidney transplantation is crucial in slowing chronic kidney disease progression (ckd progression) and reducing associated health risks.
Kidney Health and Gut Health Go Hand In Hand
The association between colon cancer and chronic kidney disease highlights the importance of understanding the risks and symptoms associated with colorectal cancer in CKD populations.
Questions about kidney transplant? Individuals with CKD, particularly those who have undergone kidney transplant or have diabetes, face a higher risk of developing colon cancer. Recognizing the symptoms such as bloody stool, persistent stomach pain, and unexplained weight loss is crucial for early detection.
By adopting healthy lifestyle habits, including maintaining a healthy weight, consuming a balanced diet, engaging in regular physical activity, refraining from smoking, and moderating alcohol consumption, individuals can potentially reduce their risk of colon cancer.
It is important to be aware of the potential risks and discuss them with healthcare providers when considering colon cancer screenings, such as colonoscopy. CKD patients should inform their doctors about their kidney function to ensure appropriate precautions are taken.
Understanding the role of uremic toxins, which are metabolic byproducts originating from intestinal microbial fermentation, further emphasizes the need for ongoing research and interventions targeting the balance of intestinal microbiota in CKD.
By staying informed and working closely with healthcare professionals, individuals with CKD can take proactive steps to address the association between colon cancer and CKD, ultimately improving their overall health and well-being.