Diet For Hemodialysis Patients
Hemodialysis (HD) is the medical method of cleaning waste and free water from your blood if your kidneys go into renal failure, and is one of three ways—kidney transplant and peritoneal dialysis being the others—in which renal replacement can be performed.
With a hemodialysis diet, there are fewer dietary restrictions than you might have to face dealing with other renal replacement treatments, but the restrictions are still there.
If you are a loved one is dealing with advanced chronic kidney disease and well into End Stage Renal Disease requiring dialysis, then it is essential that you have thorough knowledge of the special considerations of a dialysis renal diet.

Jump to:
- Key Takeaways
- Understanding Hemodialysis
- Diet Restrictions
- Recommended Foods
- Foods to Avoid
- Understanding Portion Sizes
- Beverage Choices
- Low Potassium Smoothies
- Meal Planning Tips
- Meal Planning Resources
- A Sample Meal Plan for A Hemodialysis Diet
- FAQs for Hemodialysis Diet
- A Proper Hemodialysis Diet Can Maximize Your Quality of Life
Key Takeaways
- Hemodialysis patients should eat more high quality protein foods and fewer foods high in salt, potassium, and phosphorus.
- Meal planning resources can help HD patients develop a balanced meal plan and make food substitutions using the same nutrients needed during dialysis.
- Lean meat, poultry, fish, and egg whites are allowed on a hemodialysis diet as they are high in protein and essential amino acids.
- HD patients should consult with a doctor or renal dietitian for safe beverage choices and explore low potassium smoothies as a nutritious option.
For More Recipes and Ideas --->> Get Your Free Meals and Recipes That Are Perfect for Pre-Dialysis Diets, Pre-Dialysis with Diabetes, or Dialysis Diets.
Understanding Hemodialysis
Hemodialysis is a crucial medical procedure used to treat people with kidney disease at late stages or end-stage renal disease. When the kidneys can no longer effectively filter waste products and excess fluids from the blood, hemodialysis steps in to replicate this essential function.
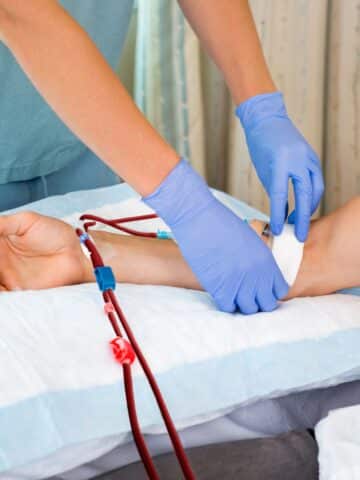
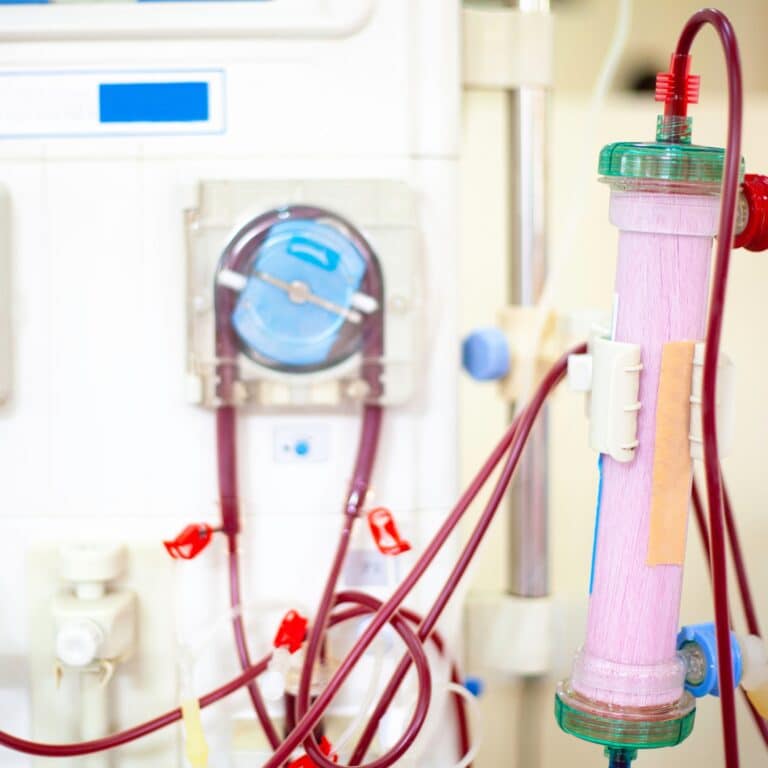
During a hemodialysis session, the patient's blood is carefully circulated outside their body and through a machine called a dialyzer. This device acts as an artificial kidney, filtering out waste, toxins, and extra fluids before returning the cleansed blood to the body.
Regular hemodialysis sessions, usually conducted multiple times a week, are essential for maintaining the body's fluid and electrolyte balance, controlling blood pressure, and preventing the buildup of harmful substances that can lead to serious health complications.
The procedure plays a vital role in improving the quality of life for those with compromised kidney function, enabling them to continue functioning despite their kidney's limitations.
Questions about kidney transplant? Hemodialysis can be a bridge to a kidney transplant or a long-term treatment option for individuals who are not suitable candidates for transplantation.
While it undoubtedly prolongs and improves the lives of many patients, hemodialysis also requires strict adherence to dietary and fluid restrictions, as well as close medical supervision, to ensure its effectiveness and the patient's overall well-being.
Diet Restrictions
A hemodialysis diet is a critical component of managing kidney failure or end stage kidney disease and ensuring the effectiveness of the hemodialysis procedure. Patients undergoing hemodialysis must adhere to specific dietary restrictions to prevent complications and maintain overall health.
Fluid Intake: Hemodialysis patients often face fluid retention due to compromised kidney function. Consequently, fluid intake must be closely monitored and restricted to avoid straining the heart and exacerbating hypertension. This fluid restriction diet is worth checking out.
Sodium Control: Excessive sodium intake can lead to fluid retention and high blood pressure. Patients are advised to limit their consumption of salty foods like processed, canned, and fast foods. How do you eat out on a low sodium diet!
Potassium Management: Impaired kidneys struggle to regulate potassium levels, which can affect heart function. Patients should limit potassium-rich foods such as bananas, oranges, potatoes, and certain meats.
Phosphorus Restriction: High phosphorus levels can lead to weak bones and contribute to heart problems. Patients must reduce intake of phosphorus-rich foods like dairy foods, nuts, and colas.
Protein Intake: While protein is necessary for muscle maintenance, excessive consumption can produce waste that the kidneys can't effectively eliminate. Protein intake is balanced to avoid waste buildup.
Caloric Control: Hemodialysis increases energy expenditure. Patients need adequate calories to prevent muscle loss and fatigue.
Micronutrient Monitoring: Vitamins and minerals might be lost during dialysis. Supplements could be recommended to prevent deficiencies.
A well-managed hemodialysis diet, tailored to individual needs and regularly reviewed by a registered dietitian, ensures that patients can optimize their overall health, complement the benefits of hemodialysis treatment, and minimize the risk of complications associated with kidney failure.

Recommended Foods
Recommended Foods for a Dialysis Diet: Dialysis kidney diets carefully designed to manage kidney function and support overall health for individuals undergoing hemodialysis. While restrictions are important, there are still plenty of nutritious options available.
High-Quality Proteins: Opt for lean protein sources like poultry, fish, eggs, and small amounts of lean meats. These provide essential amino acids while minimizing waste buildup.
Low-Potassium Fruits and Vegetables: Choose fruits like apples, berries, and grapes, and vegetables like green beans, lettuce, and cauliflower (cauliflower renal diet). These are lower in potassium, reducing the strain on the kidneys.
Low-Sodium Foods: Incorporate foods like fresh vegetables, herbs, and spices for flavor instead of salt. Opt for low-sodium or salt-free products when possible.
Grains and Starches: Enjoy moderate amounts of whole grain products like rice, pasta, and whole grain bread. These are good sources of energy and fiber.
Dairy Alternatives: Consider non-dairy milk products like almond or rice milk to limit phosphorus intake. Check food labels for added nutrients.
Limited Phosphorus Foods: Consume small portions of cheese, rice milk, or egg whites, which are lower in phosphorus.
Healthy Fats: Choose sources like olive oil, avocados, and nuts in moderation to maintain a balanced diet.
Appropriate Fluids: Consume fluid in accordance with your doctor's recommendations. Limiting intake while choosing ice chips, ice pops, or small sips of water can help manage fluid retention.
A dialysis diet aims to strike a balance between providing necessary nutrients and minimizing the strain on the kidneys. It's important to work closely with a registered dietitian or health care provider to create a personalized food plan that considers individual needs, restrictions, and preferences.
Foods to Avoid
A hemodialysis diet requires careful consideration to prevent complications and maintain the effectiveness of the treatment. Certain foods must be restricted due to their potential to exacerbate kidney issues and disrupt fluid and electrolyte balance.
High-Potassium Foods: Avoid foods rich in potassium, such as bananas, oranges, potatoes, and spinach. Excess potassium can lead to heart rhythm disturbances.
High-Sodium Foods: Steer clear of high-sodium options like processed foods, canned soups, and fast food. Sodium contributes to fluid retention and high blood pressure.
Phosphorus-Rich Foods: Limit intake of phosphorus-containing foods like dairy products, nuts, and colas. High phosphorus levels can cause bone disease and cardiovascular disease.
High-Protein Foods: While protein is essential, excessive consumption can result in waste buildup. Cut back on red meats, processed meats, and excessive protein intake.
Fluid-Heavy Foods: Avoid foods with high water content, such as watermelon and soups, as they can contribute to fluid overload.
Certain Dairy Products: High-phosphorus dairy products like cheese and yogurt should be consumed in moderation or replaced with lower-phosphorus alternatives.
Fast Foods and Processed Snacks: These often contain excessive sodium, phosphorus additives, and unhealthy fats. Fast foods that are okay for kidney disease.
Dark Colas and Sugary Drinks: These beverages contain phosphorus additives and contribute to fluid retention.
A well-balanced hemodialysis diet focuses on nutrient intake while limiting substances that strain the kidneys and disrupt fluid and electrolyte balance. Close collaboration with a registered dietitian or health care provider is essential to tailor the diet to individual needs, promote overall health, and enhance the benefits of dialysis treatments.

Understanding Portion Sizes
Portion control is a vital aspect of a hemodialysis diet, ensuring that individuals with kidney failure maintain a balanced nutrient intake while minimizing the strain on their compromised kidneys.
Managing portion sizes helps prevent the accumulation of waste products, maintains fluid balance, and supports overall well-being.
Understanding portion sizes can seem like a real challenge, but imagine it this way: your plate is a canvas where half of it should feature colorful vegetables, one quarter can be filled with carbohydrate-rich foods like pasta or rice, and the final quarter should showcase high-quality protein such as chicken or fish. This visual guide helps to ensure nutrient balance in every meal you prepare for HD patients.
For proteins like lean meats, poultry, fish, and dairy, proper portion sizes are crucial. Serving sizes should be controlled to prevent excessive protein intake, which can lead to waste buildup. Additionally, lean protein sources are favored to minimize fat consumption.
When it comes to carbohydrates, whole grains like rice, pasta, and bread should be measured to control caloric intake. Portioning carbohydrates helps prevent excess energy and supports a balanced diet.
Fruits and vegetables, especially those with high potassium content, need to be portioned carefully to avoid overwhelming the kidneys. Opting for low-potassium options and consuming them in controlled amounts helps maintain electrolyte balance.
Sodium intake should be regulated by being mindful of portion sizes in processed and packaged foods, which often contain hidden high-sodium content.
Effective portion control in a hemodialysis diet is achieved by working closely with a registered dietitian and health professionals. Customized portion guidelines based on individual nutritional needs, medical history, and treatment plan are crucial for promoting optimal health, managing kidney function, and maximizing the benefits of dialysis treatment.
Beverage Choices
Beverage choices play a pivotal role in managing fluid balance (fluid restricted diet menu) and kidney function for individuals on a renal diet. Kidney-related issues can lead to impaired fluid regulation, making it essential to monitor fluid intake closely.
Fluid Restrictions: Those on a renal diet must adhere to fluid restrictions set by their healthcare team. Limiting fluid intake helps prevent fluid overload, which can strain the heart and exacerbate hypertension. It's crucial to factor in not only beverages but also foods with high water content like fruits and soups.
Beverage Choices: Opt for hydrating options that align with fluid restrictions. Water remains a primary choice, and drinking in small sips throughout the day is encouraged. Herbal teas and caffeine-free beverages can also be enjoyed in moderation. However, it's essential to avoid dark colas and sugary drinks due to their phosphorus and potassium content. Check out these kidney friendly drinks.
Limiting Sodium: Beverages high in sodium, such as certain sports drinks and canned soups, should be avoided to maintain fluid balance.
Monitoring Electrolytes: Carefully select beverages to manage potassium and phosphorus levels. Choose low-potassium and low-phosphorus options to prevent imbalances.
Individualized Approach: Fluid restrictions can vary based on a person's specific health needs, stage of kidney disease, and other factors. Collaborating closely with a registered dietitian helps tailor beverage choices and fluid intake to ensure optimal hydration, maintain kidney health, and support the overall success of renal treatment.
Low Potassium Smoothies
After exploring various beverage options suitable for your kidney health, let's dive into a refreshing alternative: low potassium smoothies. These delightfully cool concoctions can pack a nutritional punch and offer much-needed variety to your renal diet.
Low potassium fruits are the key ingredients here. Apples, berries, and peaches make excellent choices that won't overload you with potassium. For an additional protein boost, consider adding high-quality protein sources like Greek yogurt or protein powder approved by your renal dietitian.
Crafting these kidney-friendly beverages isn't just about picking the right fruits and protein; it's also about avoiding ingredients high in potassium - bananas and oranges are commonly used in smoothies but should be avoided on a hemodialysis diet. Don't worry though! There are plenty of other flavor combinations to explore.
Remember that meal planning tools are invaluable resources when navigating dietary restrictions, helping you keep track of necessary nutrients while limiting those harmful in excess amounts. Your renal dietitian is another crucial part of this journey; their assistance ensures you're making choices that support kidney health without sacrificing taste.
So go ahead, whip up a delicious low-potassium smoothie today! It's one more step towards maintaining balance in your hemodialysis diet while enjoying the diverse flavors at hand.
Meal Planning Tips
Meal planning and prepping are essential strategies for individuals following a hemodialysis diet, ensuring they adhere to dietary restrictions while enjoying balanced and nutritious meals.
- Consult a Dietitian: Collaborate with a registered dietitian specializing in renal nutrition to develop a personalized food plan tailored to your dietary needs, preferences, and treatment regimen.
- Portion Control: Measure and portion foods according to your dietitian's recommendations. Portion control prevents overconsumption of nutrients that may strain the kidneys.
- Focus on Nutrient Density: Opt for nutrient-rich foods that provide essential vitamins and minerals without excessive potassium, phosphorus, sodium, or protein. Include lean proteins, whole grains, and low-potassium fruits and vegetables.
- Balanced Plate: Aim for a balanced plate with half filled with non-starchy vegetables, a quarter with lean protein, and a quarter with whole grains or starches.
- Meal Prepping: Prepare meals in advance to maintain consistency. Portion and pack meals that align with your dietary requirements. Use containers to separate high-potassium ingredients to control portions.
- Snack Smartly: Have kidney-friendly snacks like apple slices, carrot sticks, or a handful of nuts readily available to avoid reaching for forbidden foods.
- Hydration Planning: Monitor fluid intake, including soups, fruits, and beverages. Distribute fluid consumption evenly throughout the day and follow fluid restrictions.
- Label Foods: Label containers with dates and notes to ensure freshness and adherence to dietary guidelines.
- Stay Informed: Keep up with dietary recommendations and new recipes to maintain variety and enjoyment in your meals.
- Adapt and Learn: Be open to learning and adapting your food plan based on feedback from your healthcare team and your body's response to the diet.
A well-thought-out meal plan and strategic meal prepping can help individuals on a hemodialysis diet manage their nutritional needs, minimize kidney strain, and enhance their overall well-being.
Meal Planning Resources
After considering those important meal planning tips, it's crucial to dive into the vast array of resources available to further support your dietary journey. Remember, you're not alone in this; there are countless tools and professionals ready to help you manage your diet specifically for hemodialysis.
- Online Resources: A quick internet search can reveal a treasure trove of meal planning guides and interactive tools aimed towards understanding sodium intake and maintaining a balanced kidney-friendly diet.
- Renal Dietitian Consultation: Your renal dietitian is an invaluable source of personalized recommendations tailored to your specific needs. They can guide you on low sodium spices, calorie boosting foods, and much more.
- Nutrition Labels: Get into the habit of reading nutrition labels on packaged foods. This simple practice will help you identify high-sodium or potentially harmful ingredients quickly.
- Kidney Health Books & Magazines: These publications often contain valuable information, including recipes that align with hemodialysis dietary restrictions.
Remember, managing your food intake while on dialysis doesn't mean sacrificing taste or variety in your meals. With these resources at hand and constant learning about dietary modifications necessary for HD patients, you are well-equipped to maintain both healthful living and enjoyable eating experiences.
A Sample Meal Plan for A Hemodialysis Diet
Based on examining several kidney disease research and diet resources, if your doctor or renal dietitian has decided you should have restricted potassium, phosphorus, and fluid restrictions, one sample menu plan for a hemodialysis diet could resemble this:
Breakfast—A breakfast sandwich consisting of scrambled egg whites with two ounces of thin-sliced meat on toast or an English muffin, and four ounces of non-acidic fruit juice. Check out this renal diet breakfast lunch dinner.
Lunch—A salmon or other fish salad consisting of a cup of romaine lettuce, an eighth of a cup of raw broccoli, a tablespoon of slivered or chopped nuts, three ounces of cooked salmon, and low-fat dressing, with a small white roll buttered with trans-fat-free margarine on the side, and a four-ounce glass of a water or non-carbonated beverage.
Snack—Low sodium or sodium-free Ritz crackers with low-sodium cream cheese.
Dinner—Three ounces of grilled skinless chicken, half a cup of squash, half a cup of cabbage atop a cup of cooked pasta, substituting two tablespoons of olive oil and half a cup of low-sodium chicken broth for pasta sauce, half a cup of cherries, and a four-ounce glass of water, with orange sherbet for dessert.
FAQs for Hemodialysis Diet
The hemodialysis process significantly impacts a patient's nutritional needs due to its effects on waste elimination, fluid balance, and nutrient loss. Hemodialysis removes waste products, including excess nutrients, from the bloodstream. As a result, patients require higher protein intake to counter protein loss during dialysis.
Fluid restriction is crucial to prevent fluid overload and hypertension. Reduced kidney function can lead to imbalances in electrolytes like potassium and phosphorus, necessitating controlled intake.
Overall, the hemodialysis procedure demands a tailored diet plan to maintain proper nutrition, minimize complications, and support the patient's overall health and well-being.
A hemodialysis diet differs from a regular healthy diet due to its stringent restrictions on certain nutrients. Hemodialysis patients must monitor potassium, phosphorus, sodium, and fluid intake more closely to prevent imbalances that compromised kidneys can't regulate. Protein intake is adjusted to minimize waste buildup while maintaining muscle health.
Additionally, portion sizes are controlled to prevent strain on the kidneys. Unlike a typical healthy diet, a hemodialysis diet is personalized, focusing on nutrient management to accommodate the specific needs of kidney function, fluid retention, and waste elimination, while still aiming to provide essential nutrients and maintain overall health.
Failure to adhere to a proper hemodialysis diet can lead to various health complications. Excessive fluid intake can cause fluid overload, leading to heart strain and high blood pressure. High potassium and phosphorus levels can result in heart trouble with irregular heartbeats, muscle cramps and muscle weakness, and bone problems.
Consuming too much protein may increase buildup of waste products, causing nausea, fatigue, and even potential heart and kidney strain. Additionally, disregarding sodium restrictions can lead to fluid retention and hypertension.
Neglecting the specialized dietary guidelines of a hemodialysis diet can exacerbate kidney-related issues, compromise overall health, and increase the risk of cardiovascular disease and other complications.
Yes, specific dietary supplements are often recommended for patients on hemodialysis to address potential deficiencies. Common supplements include water-soluble vitamins like B-complex vitamins (B1, B2, B6, B12), vitamin C, and folic acid, as these are lost during dialysis.
Vitamin D and calcium supplements may be advised to maintain bone health. Iron supplements can counteract anemia, a common issue in dialysis patients.
However, these supplements should only be taken under medical supervision to prevent overconsumption, interactions, and potential harm. A registered dietitian or healthcare provider tailors supplementation to individual needs based on blood test results and dietary intake assessment.
Yes, a vegetarian or vegan (vegan renal diet) can follow a hemodialysis diet while meeting their nutritional needs, but careful planning is essential. Plant-based sources of protein like legumes, tofu, tempeh, and seitan can replace animal protein while providing essential amino acids.
However, managing potassium and phosphorus intake becomes more critical, as many plant-based foods are high in these minerals.
Careful portion control and choosing lower-potassium and lower-phosphorus options are crucial. Consulting a registered dietitian with expertise in renal nutrition can help design a well-balanced vegetarian or vegan hemodialysis diet that addresses nutrient needs while respecting dietary preferences and restrictions.
A Proper Hemodialysis Diet Can Maximize Your Quality of Life
A hemodialysis diet is pivotal in managing kidney failure and optimizing hemodialysis effects. Balancing nutrients, fluid intake, and electrolytes is key. Focus on quality protein, low-potassium produce, and low-sodium foods, avoiding high-potassium and high-phosphorus items.
Portion control is vital. Registered dietitian collaboration is crucial for personalized plans.
Hydration choices impact fluid balance; adhere to limits while choosing water and herbal teas. Low-potassium smoothies (smoothies for kidney disease) offer variety. Planning and prepping aid adherence. Resources like online tools and dietitian consultations enhance meal planning.
A well-managed hemodialysis diet, guided by professionals and individualized, improves health, minimizes issues, and aids kidney failure and hemodialysis challenges.
Did you find this information useful? Please pass it along!