Questions About Dialysis
Dialysis is one of the two options for people who have reached end stage renal disease. Once your kidneys have lost enough function, patients need either dialysis or kidney transplant to replace their failed kidneys. You cannot live with completely failed kidneys, which is why either dialysis or transplant is required.
In this article, we will answer some of your pressing questions regarding dialysis.
Jump to:
- Key Takeaways
- What Is Dialysis?
- What Are The Types of Dialysis?
- What is the Function of Dialysis?
- What are the Benefits of Dialysis?
- When is Dialysis Necessary for Renal Disease?
- What are the Alternatives to Dialysis?
- Hemodialysis Vs Peritoneal Dialysis
- What Are Location Options for Dialysis Procedures?
- What Is Home-Based Dialysis Like?
- What Is Dialysis in Hospitals Like?
- How Frequent are Dialysis Sessions Done?
- What Lifestyle Changes Are Necessary for Dialysis?
- Why Is It Important to Undergo Regular Dialysis?
- Does Dialysis Hurt?
- Dialysis May Be Daunting, But Knowledge Can Help
Key Takeaways
- Dialysis is a medical procedure that replaces the function of the kidneys.
- There are two types of dialysis: hemodialysis and peritoneal dialysis.
- Dialysis helps remove waste and excess materials in the blood, maintain electrolyte balance, control blood pressure, and remove excess fluid from the body.
- Dialysis is necessary for people with end stage renal disease, when transplant is not an option or has long waiting lists, and helps maintain overall health and well-being.
For More Recipes and Ideas --->> Get Your Free Meals and Recipes That Are Perfect for Pre-Dialysis Diets, Pre-Dialysis with Diabetes, or Dialysis Diets.
What Is Dialysis?
Dialysis is a medical procedure employed to support individuals with impaired kidney function due to chronic kidney disease (CKD), particularly for people with kidney failure or end-stage renal disease (ESRD).
When the kidneys cannot effectively filter waste products and excess fluids from the blood, the dialysis machine acts as an artificial substitute. This life-sustaining process helps maintain a balance of electrolytes and fluids in the body, regulates blood pressure, and removes toxins that healthy kidneys would typically eliminate.
Dialysis involves the use of specialized equipment to cleanse the blood, mimicking the kidney's natural filtration function. Regular sessions of dialysis are crucial for individuals with compromised kidney function to sustain their overall health and manage critical aspects of bodily function that are normally regulated by the kidneys.
What Are The Types of Dialysis?
Dialysis, a life-sustaining medical procedure, is primarily divided into two types: hemodialysis (HD) and peritoneal dialysis (PD). There will be many factors to consider when deciding which type of dialysis may be best for you.
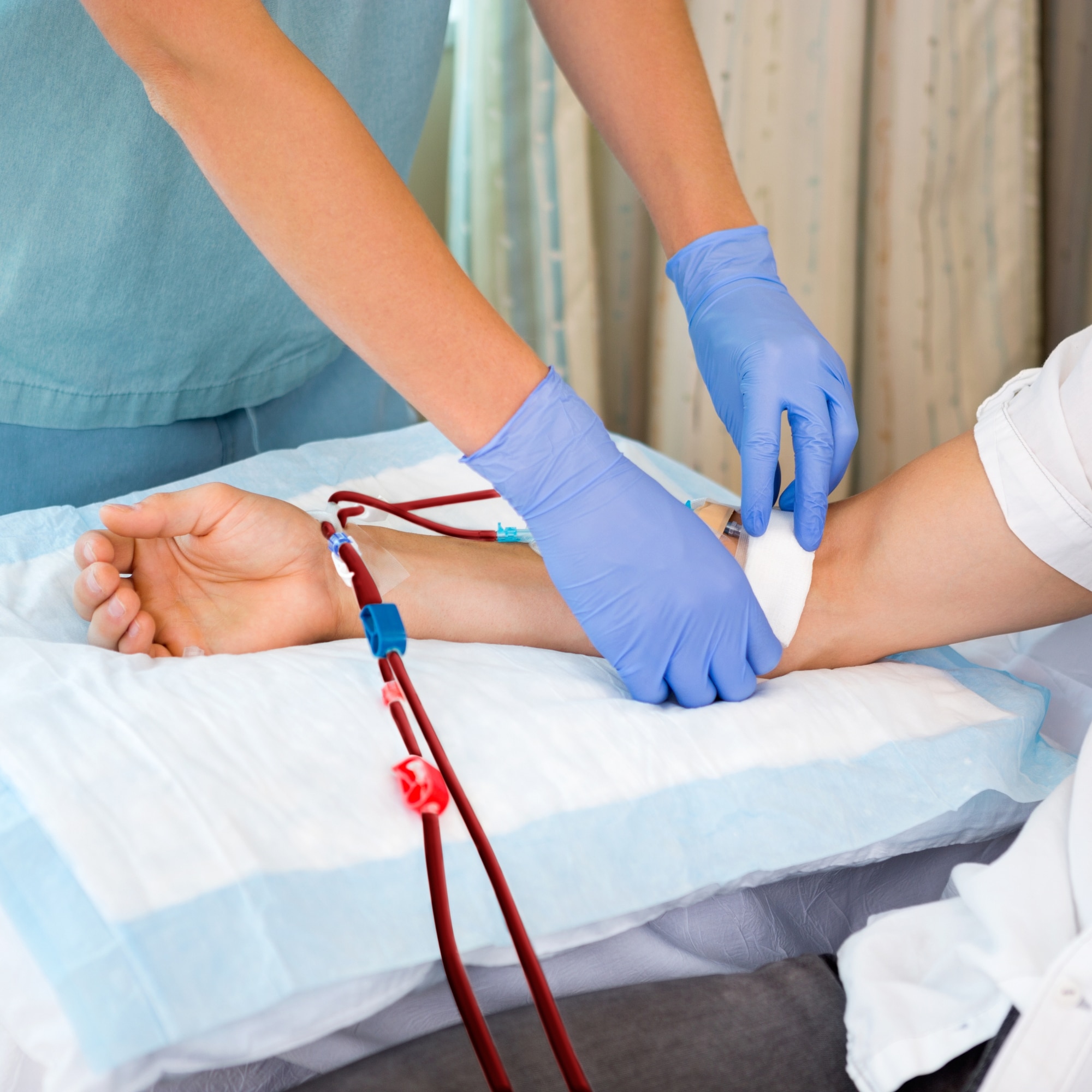
Hemodialysis involves rerouting a patient's blood through an external filter, called a dialyzer, which eliminates waste products and excess fluids before returning the cleansed blood to the body. Typically conducted at a dialysis clinic, hemodialysis requires a vascular access point such as a catheter access an arteriovenous graft (AV graft), or AV fistula, often created surgically, to facilitate blood flow during the procedure.
In contrast, peritoneal dialysis utilizes the body's peritoneal membrane as a natural filter. A special cleansing fluid, known as dialysate, is introduced into the abdominal cavity via a catheter. Waste products diffuse from the blood vessels in the peritoneal membrane into the dialysate, which is later drained.
Peritoneal dialysis patients usually have greater flexibility, as the procedure can be performed at home, but the choice between hemodialysis and peritoneal dialysis hinges on individual health, lifestyle, and medical considerations.
What is the Function of Dialysis?
Dialysis is a life-sustaining medical procedure that replicates the kidney's essential functions when they are compromised. It plays a critical role in managing conditions like end-stage renal disease or acute kidney injury where the kidneys cannot effectively filter waste and excess fluids from the blood.
Hemodialysis involves diverting the patient's blood through a dialyzer, an artificial kidney that performs filtration, while peritoneal dialysis utilizes the peritoneal membrane within the patient's abdomen for this purpose. By mimicking the natural filtration process of the kidneys, dialysis helps maintain electrolyte balance, regulate blood pressure, and prevent the accumulation of harmful substances.
This therapeutic intervention provides a vital lifeline for individuals with impaired kidney function, enhancing their overall quality of life by averting complications associated with kidney failure.
What are the Benefits of Dialysis?
Dialysis offers significant benefits for patients experiencing kidney failure, especially in cases of end-stage renal disease.
Firstly, it serves as a life-saving intervention by effectively removing waste products, excess fluids, and electrolytes from the bloodstream when the kidneys can no longer perform this crucial function. By preventing the accumulation of harmful substances, dialysis helps maintain a balance in the body's internal environment, reducing the risk of complications such as fluid overload and electrolyte imbalances.
Additionally, dialysis contributes to improving overall well-being and quality of life in ESRD patients by alleviating symptoms associated with kidney failure, including fatigue, nausea, and shortness of breath. This therapeutic approach provides a bridge for patients awaiting kidney transplantation and becomes a crucial, regular procedure to sustain life and manage the consequences of advanced kidney disease.

When is Dialysis Necessary for Renal Disease?
Dialysis becomes imperative for individuals with kidney disease, particularly in end-stage renal disease, marked by a glomerular filtration rate (GFR) below 15 ml/min. This critical stage signifies a profound loss of kidney function, where the organs can no longer effectively filter waste products, excess fluids, and electrolytes from the bloodstream.
The accumulation of toxins and fluid imbalances can lead to severe health complications. The decision to initiate dialysis is guided by clinical symptoms, laboratory results, and the overall health status of the individual. Common indications include elevated serum creatinine, high blood urea nitrogen levels, and symptomatic manifestations like severe fatigue, nausea, and fluid overload.
Dialysis serves as a life-sustaining intervention, artificially performing the essential filtration functions of the kidneys, preventing the build-up of harmful substances and maintaining a stable internal environment. Timely initiation of dialysis is crucial to mitigate the potentially life-threatening consequences of advanced kidney disease and improve the overall quality of life for affected individuals.
What are the Alternatives to Dialysis?
Alternatives to dialysis are considered when individuals, especially those with end-stage renal disease (ESRD), are unable or choose not to undergo regular dialysis treatments.
One alternative is kidney transplantation, a surgical procedure where a healthy kidney from a living or deceased donor is transplanted into the recipient. While transplantation offers a chance for a more normal life and freedom from regular dialysis, it's contingent on finding a suitable donor and involves lifelong immunosuppressive medications.
Another alternative is conservative or supportive management, focusing on symptom control, dietary modifications, and medical interventions to manage complications without undergoing dialysis. This approach is chosen when the burdens of dialysis outweigh the potential benefits, particularly in elderly or frail individuals.
Ultimately, the choice between these alternatives and dialysis is highly individualized, taking into account the patient's overall health, preferences, and available resources. The decision often involves thorough discussions between healthcare providers, patients, and their families to determine the most appropriate and personalized course of action.
Hemodialysis Vs Peritoneal Dialysis
You might be wondering about the differences between hemodialysis and peritoneal dialysis, two primary types of dialysis that serve as lifesaving treatments for individuals with kidney failure. Let's delve into a comparison that takes into account various factors such as their effectiveness, potential complications, patient preference, and cost-effectiveness.
| Hemodialysis | Peritoneal Dialysis | |
| Effectiveness | Highly effective in waste removal, but it's time-consuming and may lead to 'dialysis hangover'. | Slightly less effective, but gentle and continuous, mimicking the natural kidney function. |
| Complications | May cause low blood pressure, anemia, and access-site infections. | May lead to peritonitis, hernias, and weight gain. |
| Patient Preference | Preferred by those who want supervision from the dialysis team or don't want to dialyze at home. | Preferred by those desiring more freedom, comfort, and control over their treatment. |
| Cost-Effectiveness | Higher due to clinic visits and professional healthcare assistance. | Lower as it can be performed at home, reducing medical and travel expenses. |
While these factors provide a general guide, it's important to remember that every patient is unique. Therefore, the choice between hemodialysis and peritoneal dialysis should ultimately cater to the individual's lifestyle, health status, and personal preference.
What Are Location Options for Dialysis Procedures?
Dialysis procedures are typically conducted in specialized facilities, and there are two primary locations: in-center dialysis units and home settings.
- In-Center Dialysis Units: These are specialized clinics or hospitals where patients visit for scheduled dialysis sessions. In-center hemodialysis is the most common form, and patients receive treatment under the supervision of trained healthcare professionals in their closest dialysis center of choice, such as the community dialysis unit. This setting ensures close monitoring and immediate access to medical assistance if needed.
- Home Dialysis: Some patients, based on their health condition and preference, may perform dialysis at home. Home renal dialysis includes both peritoneal dialysis (PD) and home hemodialysis (HHD). Patients receive comprehensive training to operate the dialysis equipment and manage the procedure independently. This option offers more flexibility in scheduling, greater comfort, and reduces the need for frequent travels to a medical facility.
The choice between in-center and home dialysis depends on individual circumstances, medical considerations, and the level of support available.
What Is Home-Based Dialysis Like?
Home-based dialysis, encompassing peritoneal dialysis (PD) and home hemodialysis (HHD), offers notable benefits and challenges.
The primary advantage is increased flexibility for patients who can integrate dialysis into their daily lives. PD involves using the peritoneum as a natural filter for fluid and waste removal, allowing patients to perform treatments independently. HHD enables scheduled hemodialysis sessions at home, providing more frequent and longer treatments.
Benefits include enhanced quality of life, fewer dietary restrictions, and reduced travel to dialysis centers. Patients often experience better blood pressure control and fluid removal. However, challenges include the need for dedicated training, self-discipline, and a suitable home environment.
Home-based dialysis requires a committed caregiver or trained family member. Successful implementation depends on careful patient selection, education, and ongoing support to ensure safety and efficacy in managing kidney failure outside a clinical setting.
What Is Dialysis in Hospitals Like?
Dialysis administration at hospitals or dialysis centers offers unique advantages and challenges. Hospitals provide a comprehensive medical environment with immediate access to emergency care and skilled medical professionals.
The stringent infection control measures in hospitals ensure a high standard of safety. However, drawbacks include limited scheduling flexibility, potential exposure to hospital-acquired infections, and a clinical atmosphere that may be less comfortable for long-term treatment.
Dialysis centers, specialized facilities focusing on renal care, offer a more patient-centric approach. Patients often experience a sense of community, receiving care alongside individuals facing similar challenges.
These centers provide a more flexible schedule, allowing patients to maintain employment or engage in regular activities. However, drawbacks may include the risk of inter-patient infections and the necessity for some patients to travel for access.
Choosing between hospital and dialysis center-based care involves considering individual health needs, lifestyle, and preferences. Collaborative discussions with healthcare providers and thoughtful consideration of the patient's overall well-being are crucial for making informed decisions about the most suitable dialysis setting.
How Frequent are Dialysis Sessions Done?
For individuals with End-Stage Renal Disease (ESRD), the standard frequency for dialysis sessions is typically three times per week, with each session lasting 3 to 5 hours. This conventional schedule is effective in managing waste products and excess fluid, providing vital kidney function support.
However, emerging alternatives, such as daily or nocturnal dialysis, offer more frequent sessions, potentially enhancing treatment efficacy. Daily dialysis involves shorter sessions conducted more often, providing continuous and gentler treatment. This approach may contribute to improved outcomes, better fluid control, and enhanced removal of toxins.
The choice between conventional and more frequent sessions depends on various factors, including the patient's health, lifestyle, and preferences. Collaborative decision-making with healthcare professionals ensures that the selected frequency aligns with the individual's specific needs and circumstances.

What Lifestyle Changes Are Necessary for Dialysis?
Individuals undergoing dialysis can make crucial lifestyle adjustments to enhance their overall well-being. Maintaining a kidney-friendly diet, low in potassium, phosphorus, and sodium, is essential. Proper fluid management, adhering to prescribed fluid restrictions, helps prevent complications like fluid overload.
Regular exercise and living an active life, tailored to individual capabilities, contributes to cardiovascular health and overall fitness. Strict adherence to medication regimens prescribed by healthcare providers is vital for managing comorbidities.
Stress management through techniques like mindfulness or meditation supports mental well-being. Establishing a consistent sleep routine fosters better rest, aiding overall health.
Engaging in open communication with healthcare professionals, attending regular medical appointments, and seeking support from dialysis health care teams or support groups are integral aspects of managing the lifestyle challenges associated with dialysis.
Making informed choices and maintaining a holistic approach to health ensures individuals on dialysis (dialysis effect on body) can lead fulfilling lives while managing their condition effectively.
Why Is It Important to Undergo Regular Dialysis?
Regular dialysis is vital for individuals with End-Stage Renal Disease (ESRD) as it replicates essential kidney functions, removing waste products and excess fluids from the body. Missing a dialysis session can lead to a dangerous accumulation of toxins, electrolyte imbalances, and fluid overload. These complications can result in severe symptoms such as fatigue, shortness of breath, nausea, and hypertension.
Furthermore, untreated fluid overload can strain the heart, leading to cardiovascular issues. Accumulated toxins can affect various organ systems, contributing to a range of complications, including neurological symptoms like confusion and, in extreme cases, seizures. The longer the gap between dialysis sessions, the higher the risk of these complications, posing immediate threats to the individual's health.
Consistent and timely dialysis sessions are crucial to sustaining life in ESRD patients. Healthcare providers carefully schedule sessions based on individual needs, and any deviation from this schedule can have severe consequences, emphasizing the critical nature of adherence to regular dialysis for maintaining stability and preventing life-threatening complications.
Does Dialysis Hurt?
Dialysis itself is generally not painful as it's performed using sterile techniques and specialized equipment. However, some patients may experience discomfort or minor pain during needle insertion at the access site, but this is usually brief. The discomfort tends to decrease with regular sessions as patients become accustomed to the procedure.
Complications of dialysis can include infections at the access site, bloodstream infections, clotting of the dialysis access, drop in blood pressure, muscle cramps, abdominal cramps, and nausea. Long-term complications may involve the development of scar tissue at the access site or the need for interventions to maintain access. Additionally, repeated needle insertions can contribute to access site pain and potential psychological stress for a person on hemodialysis.
While dialysis itself isn't inherently painful, the associated complications and potential discomfort emphasize the importance of close monitoring, preventive measures, and a collaborative approach between healthcare providers and patients to optimize the dialysis experience and overall well-being.
Dialysis May Be Daunting, But Knowledge Can Help
If you have many questions about dialysis and end stage renal disease, talk to your doctor about your concerns. You should also consider setting up a meeting with your nearby dialysis center so they can show you what dialysis looks like and how it is done.
Seeing the process in person may help alleviate any fears you may have about this life saving procedure.












It's good to learn that dialysis is basically painless since the only painful part would be the insertion of the port. Knowing this is quite reassuring for me since my dad is scheduled for a dialysis later in the day. I would hate it if he were to suffer since he's been through wars long enough. Hopefully, he'll turn out well afterward. I'll take up your advice and talk to the doctors about any other concerns I might have during his dialysis. Thanks!