How is Kidney Disease Diagnosed?
Have you ever wondered exactly how chronic kidney disease (CKD) is diagnosed? Maybe you have begun having symptoms or know a loved one that is experiencing them. Note that it's very common to experience zero symptoms of kidney disease until it has become well advanced.
With one in three Americans at risk for kidney disease, however, it is important that you understand how to find out if you have the medical condition.
If you're older, diabetic, obese, or have hypertension, it's especially important for you to keep an eye on your kidneys.
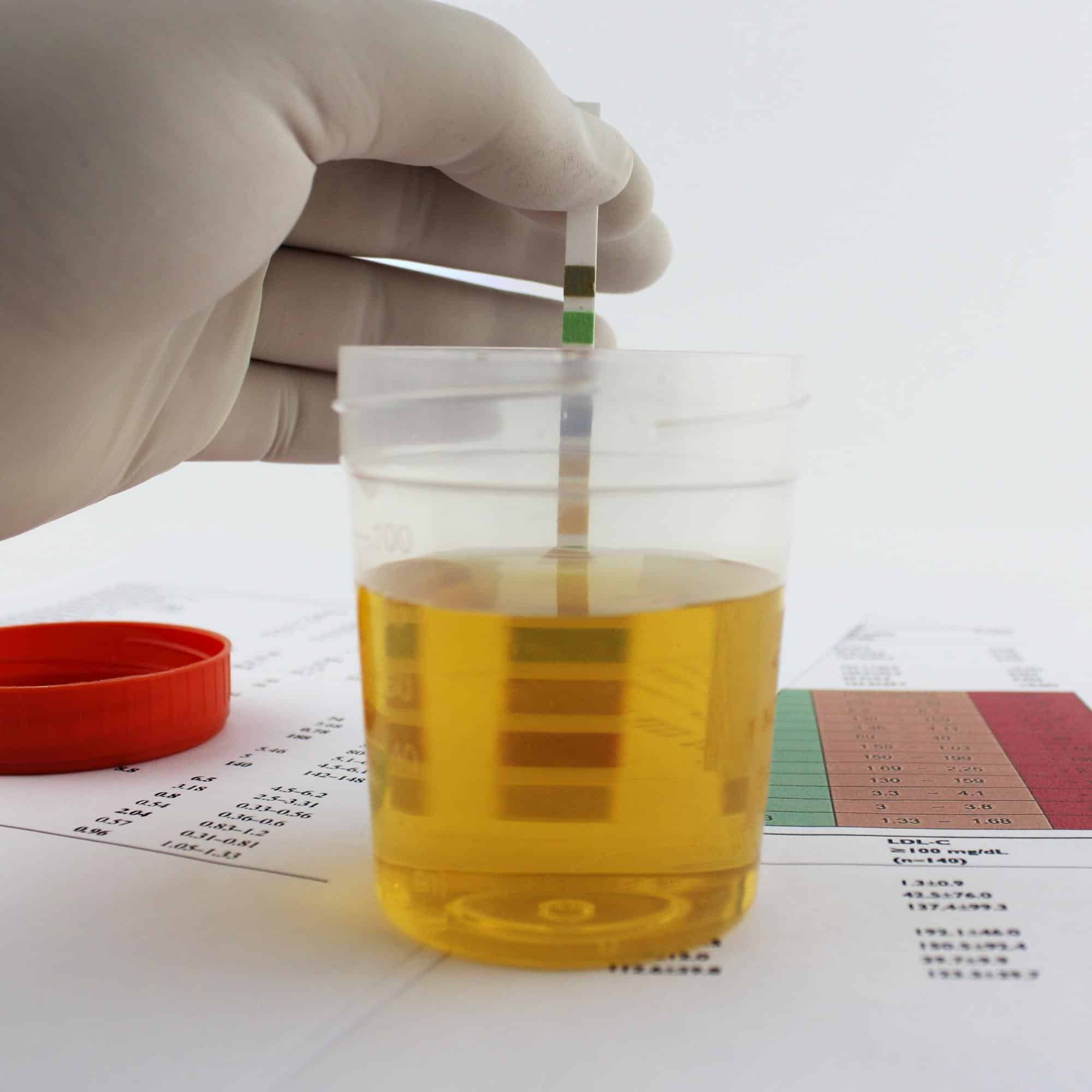
You'll learn all about the key tests used in CKD diagnosis - from urine tests measuring albumin levels to blood tests checking creatinine levels. You'll understand how these results are used to evaluate the health of your kidneys.
Ultrasounds and biopsies may also come into play for further examination. The goal? Early detection; catching CKD as soon as possible gives us the best shot at managing it effectively and slowing its progression (ckd progression).
So let's get started - knowledge is power in maintaining renal health!
Jump to:
- Key Takeaways
- Risk Factors Identification
- Family Doctor Consultation
- Importance of Routine Testing
- Urine and Blood Tests
- Understanding Ultrasound Results
- When is Kidney Biopsy Required?
- How CKD Diagnosis is Made
- Early Detection Advantages
- Treating The Underlying Cause
- Managing Complications
- Treatment for End-Stage Condition
- FAQs for Kidney Disease Diagnosis
- Early CKD Diagnosis Can Help Slow Progression and Prevent Complications
Key Takeaways
- Routine appointments with a family doctor are important for early detection and monitoring of kidney disease.
- Urine and blood tests are commonly used to diagnose kidney disease and assess kidney function.
- Imaging techniques, such as ultrasound, can be used to check for abnormalities in kidney structure and size.
- In some cases, a kidney biopsy may be performed to gather additional information about the cause of kidney issues.
For More Recipes and Ideas --->> Get Your Free Meals and Recipes That Are Perfect for Pre-Dialysis Diets, Pre-Dialysis with Diabetes, or Dialysis Diets.
Risk Factors Identification
Did you know your lifestyle and even your genetics could be silently nudging you towards chronic kidney disease? Let's dive into identifying these risk factors.
You might be surprised to learn that simple aspects of your daily life, such as weight management and physical activity, play a pivotal role in maintaining renal health. Carrying extra pounds puts a strain on your kidneys and can lead to diseases like diabetes and hypertension, which are leading causes of kidney disease.
Your genetic predisposition also matters. If a close family member has kidney disease, it increases your risk too. It's crucial to share this information with your doctor for early detection strategies.
Moreover, certain lifestyle choices need modifications. Smoking or excessive drinking? They're harmful not just for the lungs or liver but the kidneys too! And while medications help manage health conditions, some have adverse effects impacting kidney function negatively over time.
Racial disparities cannot be ignored either; African-Americans, Native Americans, or Asian-Americans face higher risks. Therefore, regular check-ups are essential if you belong to these demographics.
So remember: making proactive decisions about weight control, understanding your family history, adjusting lifestyle habits positively, and being aware of medication side effects (ckd and diabetes medications) go a long way in safeguarding against kidney disease.

Family Doctor Consultation
Routine consultations with a family doctor play a pivotal role in the prevention and early detection of chronic kidney disease. Family doctors serve as primary care providers who are well-equipped to monitor and assess various health indicators, making them instrumental in identifying risk factors and initiating timely interventions.
Regular check-ups allow family doctors to monitor blood pressure, blood glucose levels, and perform routine blood tests to assess kidney function. These indicators provide crucial insights into the health of the kidneys and can help detect early signs of CKD.
Additionally, family doctors can review medical history, assess lifestyle factors like diet and exercise, and identify any hereditary predispositions to kidney disease.
Early detection is vital in CKD, as it enables proactive measures to slow disease progression and prevent complications. Family doctors can offer guidance on maintaining a healthy lifestyle, managing underlying conditions like diabetes and hypertension that contribute to CKD, and prescribing medications to control blood pressure and protect kidney function.
Moreover, family doctors facilitate patient awareness and education about CKD risk factors, symptoms, and the importance of adherence to medical recommendations. They act as a point of contact for addressing concerns and providing ongoing support throughout a patient's healthcare journey.
Taking the time to regularly consult with your trusted family doctor, especially when it comes to discussing potential risk factors and symptoms, can make all the difference in catching health issues early on.
Importance of Routine Testing
Routine testing plays a crucial role in the prevention and diagnosis of chronic kidney disease due to its ability to identify risk factors, detect early signs of kidney dysfunction, and enable timely interventions.
Regular testing allows healthcare providers to monitor key health indicators, such as blood pressure, blood glucose levels, and markers of kidney function, even before noticeable symptoms arise.
Early detection of CKD is vital as it provides an opportunity to address underlying causes and implement strategies to slow disease progression. Routine testing also aids in identifying individuals at risk for CKD, such as those with diabetes, hypertension, or a family history of kidney disease, allowing for tailored preventive measures (meal planning for families with CKD).
Routine testing helps healthcare professionals establish baseline data, track changes over time, and make informed decisions about treatment plans. It helps in identifying fluctuations in kidney function and other potential complications, which guides the lifestyle modifications and necessary medication adjustments in patients to better manage CKD.
Furthermore, routine testing empowers individuals with knowledge about their kidney health, enabling them to actively engage in their care and make informed decisions about their lifestyle, diet, and medication adherence.
By incorporating regular testing into healthcare routines, individuals can play an active role in preventing the onset of CKD or managing its progression effectively, ultimately promoting long-term kidney health and overall well-being.
Urine and Blood Tests
Diagnosing chronic kidney disease involves a combination of urine tests and blood tests that provide valuable insights into kidney function, allowing for early detection, accurate staging, and appropriate management. These tests play a critical role in assessing kidney health, identifying potential underlying causes, and guiding treatment decisions.
Urine tests are crucial for evaluating kidney function and detecting abnormalities. A common test is the urinalysis, which examines the urine for the presence of protein, blood, and other substances. A simple urinalysis also involves examination of sediment which can provide clues for certain abnormalities such as the presence of white blood cells or cellular casts.
Proteinuria (the presence of urinary albumin or excess protein in the urine) and hematuria (the presence of blood in the urine) can be indicators of kidney damage.
Additionally, the urine albumin-to-creatinine ratio is used to quantify the amount of protein in the urine, aiding in the diagnosis of kidney disease and assessing its severity.
Blood tests are equally essential in diagnosing CKD. The serum creatinine test measures the level of creatinine in the blood, a waste product produced by muscle metabolism that is normally filtered by the kidneys.
For those with normal kidney function, there is low and stable creatinine levels in the blood. Elevated creatinine levels indicate decreased kidney function and impaired filtration rate.
The computation of estimated glomerular filtration rate from serum creatinine levels is also usually done and is used to determine the stage of CKD.
Another critical blood test is the blood urea nitrogen (BUN) test, which measures the amount of urea nitrogen in the blood. Elevated BUN levels can indicate compromised kidney function and reduced filtration capacity (how to improve bun level).
Additionally, blood tests may include measurement of serum electrolytes such as potassium, sodium, and calcium. Imbalances in these electrolytes can affect various bodily functions and are commonly seen in individuals with kidney dysfunction.
A complete blood count can also be valuable for the evaluation for anemia, which is a complication of chronic kidney disease.
Collectively, urine and blood tests provide a comprehensive picture of kidney health, helping healthcare providers diagnose CKD, determine its stage, and assess its underlying causes.
Early detection through these tests allows for timely interventions to slow disease progression, manage complications, and maintain overall well-being. Regular monitoring of these parameters is crucial for tracking the progression of CKD and adjusting treatment plans as needed.
Understanding Ultrasound Results
Kidney ultrasound imaging, also known as kidney ultrasonography, plays a vital role in diagnosing kidney disease due to its non-invasive nature, ability to provide detailed images, and its wide availability.
Ultrasound is especially valuable in evaluating the structure, kidney size, and overall condition of the kidneys, helping healthcare professionals identify various kidney-related abnormalities and diseases.
One of the primary advantages of ultrasound is its ability to detect kidney abnormalities early in the disease process. It can reveal conditions such as kidney cysts which can be either simple cysts of complex cysts, tumors, kidney stones, and obstructions in the urinary tract.
Additionally, ultrasound is effective in assessing kidney size and shape, which can be indicative of underlying kidney disorders.
Ultrasound imaging is particularly beneficial for monitoring the progression of chronic kidney disease. It allows for the visualization of changes in kidney size, blood flow, and the presence of kidney stones or other complications that can arise as CKD advances. Use these tips to understand how quickly will my chronic kidney disease progress to dialysis.
Furthermore, ultrasound is a safe and radiation-free imaging technique, making it suitable for various patient populations, including pregnant women and children. It is non-invasive and painless, involving the use of sound waves to create images of the kidneys in real-time.
Renal ultrasonography is an indispensable tool in diagnosing kidney disease as it provides accurate, non-invasive, and detailed images of the kidneys and surrounding structures.
Its ability to detect kidney abnormalities, monitor disease progression, and guide treatment decisions makes it an essential component of the diagnostic process for kidney-related disorders.
When is Kidney Biopsy Required?
Kidney biopsy involves extracting a tiny sample of kidney tissue for examination under a microscope. This procedure aids in accurate diagnosis, helping medical professionals tailor treatment plans to address the specific kidney condition.
Kidney biopsy is a diagnostic procedure that becomes necessary under specific indications to determine the underlying cause of kidney-related issues. The following scenarios often warrant a kidney biopsy:
- Microscopic Hematuria: The presence of blood in urine that is not visible to the naked eye can indicate underlying kidney problems. When persistent or recurrent, kidney biopsy helps identify the cause, such as glomerulonephritis or other kidney diseases.
- Urologically Unexplained Macroscopic Hematuria: Visible blood in urine without an apparent urological cause may indicate kidney-related issues. Biopsy can uncover the cause, such as kidney infections, stones, or tumors.
- Proteinuria: Excess protein in urine, known as proteinuria, suggests impaired kidney function. Biopsy can pinpoint the underlying kidney condition causing protein leakage, aiding in proper treatment planning.
- Nephrotic Syndrome: Nephrotic syndrome, characterized by significant proteinuria, low blood protein levels, edema, and elevated cholesterol, requires a biopsy to identify the specific kidney disorder contributing to these symptoms.
- Impaired Kidney Function: Biopsy becomes necessary when kidney function is impaired, as indicated by elevated creatinine levels. It helps identify the degree of damage and the underlying cause, guiding appropriate interventions.
- Hypertension: When hypertension is suspected to be linked to kidney problems, a biopsy can determine the extent of kidney damage and provide insights into suitable management.
The decision to perform a biopsy is based on clinical symptoms, laboratory assessment, imaging findings, and the need for precise diagnosis to ensure effective management of kidney-related concerns (how to manage chronic kidney disease).
How CKD Diagnosis is Made
Newly diagnosed with CKD? A diagnosis of chronic kidney disease is established through a combination of clinical assessment, laboratory tests, and medical history evaluation. Key factors that contribute to a CKD diagnosis include:
- Kidney Function: The hallmark of CKD is impaired kidney function, reflected in the markers of kidney damage which can be seen as elevated levels of serum creatinine, blood urea nitrogen, and reduced estimated glomerular filtration rate (eGFR). A consistent decline in eGFR over a period of three months or more is indicative of permanent loss of kidney function, which is the definition of CKD.
- Kidney Damage: Evidence of kidney damage, which can be identified through abnormalities in urine tests such as persistent proteinuria (excess protein in urine) or hematuria (blood in urine), is a crucial component of CKD diagnosis.
- Duration: A diagnosis of CKD requires that kidney damage and/or decreased kidney function persist for at least three months. Acute kidney injury (AKI) refers to a sudden decline in kidney function that is reversible, whereas CKD implies a chronic and irreversible decline.
- Staging: CKD is categorized into five stages based on eGFR levels and the presence of kidney damage, as defined by the National Kidney Foundation's Kidney Disease Outcomes Quality Initiative (KDOQI) guidelines. These stages range from mild (Stage 1) to severe (Stage 5) based on the degree of impairment.
- Underlying Causes: Establishing the underlying cause of CKD is crucial, as it guides treatment and management strategies. Common causes include diabetes, hypertension, glomerulonephritis, and polycystic kidney disease.
- Medical History: Assessing a patient's medical history, family history, and risk factors helps determine the likelihood of CKD development. Factors such as diabetes, hypertension, cardiovascular disease, and a family history of kidney disease increase the risk.
- Imaging Studies: Imaging tests such as ultrasound, CT scans, and MRI provide valuable information about kidney size, shape, and potential structural abnormalities.
A comprehensive approach that combines clinical evaluation, physical examination, laboratory results, imaging studies, and patient history is essential for establishing a definitive diagnosis of CKD. Your doctor may order additional tests if needed, depending on your condition.
Early diagnosis enables healthcare providers to initiate appropriate interventions, manage complications, prevent rapid progression of kidney dysfunction, ultimately improving patient outcomes and quality of life.
Early Detection Advantages
Catching health issues at an early stage, particularly those affecting your kidneys, offers a significant advantage in devising effective treatment strategies and preventing further complications.
It's here that the role of your family doctor becomes pivotal. They not only help you understand ultrasound results but also guide you through necessary lifestyle changes.
Early detection of kidney disease enables us to:
- Establish a treatment plan.
- Slow down the progression to dialysis with End Stage Kidney Disease.
- Prolong a relatively healthy life.
These advantages stem from identifying risk factors such as diabetes, hypertension, or obesity via routine testing and diligent tracking of any symptoms or changes in urine output or color.
These benefits highlight why it is crucial to have regular appointments with your family doctor, who plays an instrumental role in early diagnosis.
Remember, successful management of chronic kidney disease hinges on understanding the importance of risk factor identification and interpreting test results accurately - all part and parcel of the benefits derived from routine testing.
So make sure to keep communication lines open with your healthcare provider for optimum renal health maintenance – because when it comes to protecting your kidneys, every second counts!
Treating The Underlying Cause
Treating the underlying cause of chronic kidney disease is crucial for managing the condition and slowing its progression. CKD can result from various factors such as diabetes, hypertension, glomerulonephritis, and more. Addressing the root cause can significantly impact the course of the disease.
- Diabetes Management: For diabetic kidney disease, maintaining optimal blood sugar levels is vital. This involves a combination of medication, insulin therapy, dietary modifications, and regular monitoring to prevent further kidney damage.
- Hypertension Control: High blood pressure is a common cause of CKD. Effective management through lifestyle changes and medications can help protect kidney function and prevent worsening kidney damage.
- Immune System Regulation: In cases of CKD caused by immune system disorders like glomerulonephritis and other immune glomerular disease, medications to suppress the immune response may be prescribed to reduce inflammation and slow kidney deterioration.
- Infection Treatment: Infections, especially in the urinary tract or kidneys, can lead to CKD. Treating infections promptly with antibiotics can prevent kidney damage.
- Obstruction Resolution: Kidney stones or structural abnormalities causing urine flow obstruction may lead to CKD. Removing obstructions through procedures or surgeries can prevent further harm.
- Medication Adjustments: Some medications can cause kidney damage. Among these are Nonsteroidal Anti-Inflammatory Drugs or NSAIDs. Adjusting or discontinuing these medications, under medical supervision, can help prevent further decline.
- Lifestyle Modifications: Dietary changes, exercise, weight management, and avoiding smoking and excessive alcohol consumption contribute to managing underlying causes and improving overall kidney health.
- Regular Monitoring: Consistent medical follow-up, including routine blood tests, urine analysis, and imaging, allows healthcare providers to track kidney function, adjust treatments, and intervene as needed.
Treating the underlying cause of CKD requires multidisciplinary medical care involving nephrologists, primary care physicians, dietitians, and other specialists. Customized treatment plans address both the primary cause and associated risk factors, aiming to slow disease progression, preserve kidney function, and enhance the patient's overall quality of life.
Managing Complications
Chronic kidney disease (CKD) often leads to various complications that can significantly impact a person's health and quality of life. Effective management strategies are crucial to mitigate these complications and improve overall well-being.
- Cardiovascular Complications: CKD itself is a cardiovascular risk factor, increasing the risk for heart disease, heart attacks, and strokes due to factors like high blood pressure load and fluid imbalance. Managing blood pressure, cholesterol and lipid levels, and avoiding excess fluid intake, along with adopting a heart-healthy diet and regular exercise, can reduce these risks (ckd and heart disease).
- Anemia: CKD can lead to reduced production of red blood cells and anemia. Treatment options include medications to stimulate red blood cell production (erythropoiesis-stimulating agents), iron supplements, and addressing underlying causes.
- Bone and Mineral Disorders: Imbalanced mineral levels (phosphorus, calcium, and parathyroid hormone) can weaken bones and lead to vascular calcifications. Medications, dietary adjustments, and phosphorus binders help manage these imbalances.
- Fluid Retention and Edema: Impaired kidney function can result in fluid retention, causing edema (swelling) especially at later stages such as End Stage Renal Disease. Monitoring fluid intake and adhering to prescribed fluid restrictions can prevent this complication.
- Electrolyte Imbalances: CKD disrupts electrolyte balance, leading to complications like muscle cramps, heart arrhythmias, and nerve dysfunction. Dietary modifications, medications, and regular monitoring can address these imbalances.
- Uremia: Accumulation of waste products in the blood (uremia) can lead to symptoms like fatigue, nausea, vomiting, and cognitive impairment. Dialysis or kidney transplant may be needed in advanced cases.
- High Blood Pressure: CKD often raises blood pressure, which worsens kidney damage and cardiovascular risks. Blood pressure medications, sodium restriction, and lifestyle changes help manage hypertension.
- Proteinuria: Excess protein in the urine can indicate kidney damage. Treatment focuses on addressing the underlying cause and managing protein intake.
- Infections: CKD weakens the immune system, making individuals more susceptible to infections. Preventive measures like vaccination, hygiene practices, and early treatment of infections are essential.
- Neuropathy and Muscle Weakness: Nerve damage and muscle weakness can occur. Adequate nutrition, physical therapy, and regular exercise can help manage these complications.
- Depression and Anxiety: Coping with a chronic condition can lead to mental health challenges. Psychological support, counseling, and stress management techniques are vital for emotional well-being.
Effective management of CKD complications requires a collaborative approach involving nephrologists, healthcare providers, dietitians, and other specialists. Tailoring treatment plans to individual needs, monitoring regularly, and addressing complications promptly can enhance the patient's quality of life and minimize the impact of CKD-related challenges.
Treatment for End-Stage Condition
How to prevent end stage renal disease? End-stage renal disease (ESRD) is a severe and irreversible condition where the kidneys have lost nearly all their function. Two primary treatment options for ESRD are kidney transplant and dialysis.
Kidney Transplant: A kidney transplant involves surgically replacing a failed kidney with a healthy donor kidney. It is considered the optimal treatment for ESRD, as it provides the best chance for improved quality of life and survival. Transplants can be from living or deceased donors.
A successful transplant restores kidney function, reducing or eliminating the need for dialysis. However, finding a suitable donor and managing potential organ rejection require careful assessment and lifelong immunosuppressive medications.
Dialysis: Dialysis is a life-saving treatment that mimics the kidney's function by filtering waste, excess fluids, and electrolytes from the blood. There are two main types of dialysis:
- Hemodialysis: Blood is cleansed outside the body through a dialysis machine, typically done at a dialysis center or at home with proper training. It usually involves three to four sessions per week, lasting several hours.
- Peritoneal Dialysis: The peritoneum lining the abdomen acts as a natural filter. Dialysis fluid is introduced into the abdominal cavity, allowing waste to be absorbed by the fluid and then drained out. It offers more flexibility as it can be done at home and does not require a machine.
Choosing between transplant and dialysis depends on factors such as patient health, age, medical history, donor availability, and personal preferences. Transplants offer better long-term outcomes, but they depend on donor availability.
Dialysis is a viable option for patients who are not transplant candidates or awaiting a suitable donor. Careful consideration and collaboration with healthcare professionals are vital to determine the best treatment approach for each ESRD patient.
FAQs for Kidney Disease Diagnosis
Early symptoms of chronic kidney disease can be subtle and may include fatigue, decreased appetite, and changes in urination patterns like increased frequency or foamy urine.
As CKD progresses, symptoms can intensify, leading to extra fluid retention with swelling in the ankles, feet, and hands, itchy skin, muscle cramps, and difficulty concentrating.
High blood pressure and anemia (anemia and dialysis) may also develop. Since early CKD symptoms are nonspecific, they often go unnoticed. Regular check-ups and screenings are essential, especially if you have risk factors like diabetes, hypertension, or a family history of kidney disease.
Detecting CKD early allows for timely interventions to slow progression and manage complications.
Chronic kidney disease can significantly impact overall health and daily life. As kidney function declines, waste and fluid buildup can lead to fatigue, loss of appetite, swelling, and changes in urination. Complications like anemia, bone weakness, and cardiovascular issues may arise.
CKD also affects electrolyte balance, leading to muscle cramps and irregular heartbeats. Dietary restrictions become necessary, impacting food choices and meal planning. Managing medications and adhering to treatment regimens become routine. Emotional well-being may be affected due to the life-altering nature of the disease.
Regular medical appointments become crucial. Early detection, lifestyle adjustments, and proper medical kidney care can help mitigate CKD's impact, improving quality of life and slowing disease progression.
Yes, individuals with chronic kidney disease often require dietary adjustments. Controlling intake of sodium, potassium, phosphorus, and protein is vital. Reduced sodium helps manage blood pressure, while limiting high-potassium foods prevents heart rhythm disturbances.
Monitoring phosphorus intake is crucial to prevent bone issues. Protein intake must be balanced to prevent strain on the kidneys. Fluid intake may also be restricted to manage fluid balance.
Consulting a registered dietitian is essential to create a personalized dietary plan that aligns with CKD stage and individual health needs, supporting kidney function and overall well-being.
Chronic kidney disease progresses through stages based on the estimated glomerular filtration rate and presence of kidney damage. Stages range from 1 (mild kidney damage with normal function) to 5 (end-stage renal disease, ESRD or kidney failure).
As CKD advances, kidney function gradually declines, leading to increased waste buildup, fluid imbalance, and electrolyte disruptions. Symptoms become more pronounced in later stages, including fatigue, swelling, and difficulty concentrating. Regular monitoring of eGFR, blood pressure, and kidney function markers is essential.
Early detection and management in the earlier stages can help slow progression, delay complications, and enable informed decisions about treatment options like dialysis or kidney transplant.
Numerous support resources are available for individuals with chronic kidney disease (CKD) and their families. Renal clinics, patient associations, and online platforms offer educational materials, counseling, and peer support groups to address physical, emotional, and lifestyle challenges.
Nephrologists, dietitians, social workers, and psychologists form a comprehensive care team. Medicare and private insurance cover medical expenses. Transplant centers offer information on kidney transplantation.
Dialysis centers provide training and support for in-center or home dialysis. Engaging with these resources can empower patients and families to manage CKD effectively, make informed decisions, and improve their quality of life throughout their journey.
Early CKD Diagnosis Can Help Slow Progression and Prevent Complications
Understanding the diagnostic process for chronic kidney disease is essential. Routine urine and blood tests detect risk factors and assess kidney function. Family doctor consultations and ultrasound imaging aid in early detection. Kidney biopsies help diagnose specific indications like hematuria, proteinuria, and impaired kidney function.
Questions about kidney transplant? Early detection enables tailored treatments and complication prevention. Treating CKD's underlying cause, managing complications like cardiovascular issues and anemia, and considering kidney transplant or dialysis for end-stage renal disease (ESRD) are essential.
Collaboration among healthcare providers and informed decision-making by patients play a crucial role in CKD diagnosis, management, and treatment for improved kidney health and quality of life.