Delicious Meal Plans for Kidney Health
Healthier Kidneys In Minutes A Day
Without Medicine, Without Costly Doctor or Specialist Visits, and While Avoiding Dialysis...
Meal Plans Designed By Mathea Ford, Registered Dietitian Nutritionist, Food Lover, and Author of “Living With Chronic Kidney Disease: Predialysis” and “Create Your Own Kidney Diet: Stage 3 & 4″ and "The Kidney Friendly Diet Cookbook: Recipes For A Pre-Dialysis Kidney Disease Lifestyle" On Amazon…
It's Understandable To Be Concerned About The Symptoms Of Kidney or Renal Disease ...
Whether you are taking care of a loved one with renal disease or you're worried about your own symptoms of kidney disease
But kidney disease doesn’t have to be a problem anymore

And you DON'T have to live the rest of your life eating bland, boring food! PLEASE don't spend your life eating bland, boring food
You can get healthier kidneys just by changing your diet.
I am an Army Veteran, so I am all about BLUF (Bottom Line Up Front)
After much feedback about cost and value, I have created a 2 PERSON meal plan that is flexible, adjustable, affordable and economical for all - including people on a fixed income. This is about togetherness and community and I am choosing to sell this at a VERY LOW price because I want everyone to feel that they can make the changes and improve their health. This is for YOU.
I have created a meal plan that:
- Is for 3 meals a day (and snacks depending on the calorie amount chosen) - entrees, sides, fruit, vegetables, and desserts FOR 2 PEOPLE!!! But you can adjust it and make it for 4 or more people if you want.
- Is flexible so you can change any meal, recipe, item, or entire plan for how you want it to be - servings, portions, and ingredients
- Shows you the nutritional information that you NEED and WANT to know: Calories, Carbs, Protein, Fat, Potassium, Sodium, Phosphorus and more
- Whenever you change the meal plan (any recipe in the meal plan) - it automatically updates the nutrition information
- If you don't like something - swap it out - over 300+ recipes to choose from and I continue to add to the meal plans and change them for the seasons
- Recipe that you want is not there? Add it yourself and the nutrition information is automatically added and you can add it to your plan - or send it to me and I will add it for everyone to share.
- Works online perfectly, no need to print and you can use it on your phone and / or tablet. OR update your plan and print it out for yourself. Your changes are saved as you make them so you don't have to print it out if you don't want to.
- Designed with a 1500 or 2000 calorie option - you choose and you adjust for the calories and other nutrition information you want
- BASICALLY - it's a done for you plan that you can use now or you can customize and see how it fits your plan and desires
- Don't want eggs, don't want onions, don't want [insert food here] - remove it - and I can place a notification on your account that will warn you when a recipe contains the food you don't want (or have an allergy to)
- Grocery lists, printed recipes, printed meal plans - it's all there for you to use and all adjusts when you change something in the recipes
- It's priced so that EVERYONE can access it and create their healthy meals for their specific needs
- AGAIN - you can change the recipes, meals and snacks to match your personal restrictions and even adjust for other conditions
SO IF YOU ARE READY TO CHANGE YOUR LIFE -- CLICK ON THE BUTTON BELOW FOR THE CALORIE PLAN THAT MEETS YOUR NEEDS
[If you choose the wrong one, let me know and I can switch you to the other plan, no problem]
***** You will be taken to a sister site that will allow you to purchase and manage your meal plans *******
Meal plans are $19.99/month [Introductory price] and you lock in your price for the meal plan (until you cancel)
{Not Convinced?} Keep Reading For More Information
Being someone who has kidney disease (or caring for a loved one), you know how frustrating it is when the doctor says - "Follow a low protein and low salt diet".
Most people understand those guidelines in theory but the doctors very seldom explain to you HOW to do that. So you go home and you feel helpless and confused.
Simple rules like - "Stop eating red meat" or "eat more vegetables" are nice guidelines but not really clear enough to follow for a long time. How on earth do you do that while keeping up with everything else in life?
You need a plan
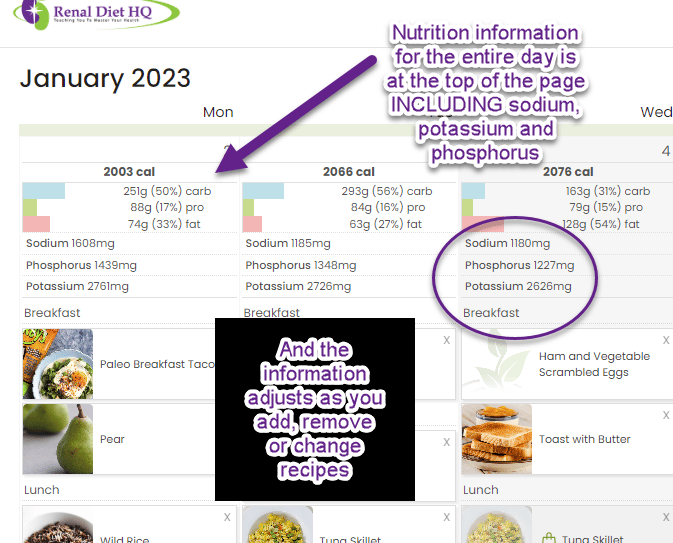
I decided then to make it my mission to help people by creating a meal plan that fits around real life and time constraints - and yet tastes yummy too.
The Solution: Delicious Meal Plans for Kidney Health
Designed as a pre-dialysis meal plan for real people living in the REAL WORLD, this plan meets the guidelines to make it a renal diet, but it does not limit you to tasteless, boring meals.
This weekly meal plan with recipes will help you to control your protein intake and you'll feel full all day!
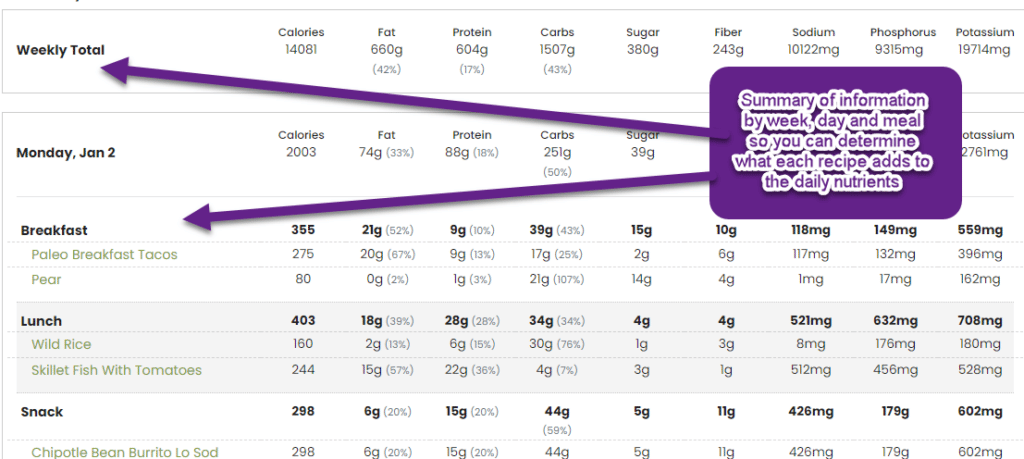
By following our menu plan, you can make your doctor happy (and your family too!) and help meet your medical care goals - which should mean less complications and medications in the long run.
It will save you time and it will give you what you need to eat to succeed at controlling your blood urea nitrogen (BUN) and creatinine.
What Do You Get With The Renal Diet Meal Plan and Recipes?
You'll Get All This Tasty Goodness Every Week!!
- 7 NEW Delicious Days Of Recipes for Kidney Health Each Week -- Breakfast Lunch and Dinner +++ Snacks
- Recipes from a a Variety of Entrees. Choose Based on What You're In the Mood for Or What's On Sale - Beef, Fish, Chicken, Turkey, Pork and Vegetarian
- Recipes For Side Dishes to Accompany the Entrees and Create a Complete Day! And more recipes to choose from
- Nutritional Information For Meals. Calories, protein, carbohydrate, potassium, phosphorus, sodium and more that changes when you change your meals!
- Grocery List For The Week of Meals By Section Of The Grocery Store - Easy to Use By You Or Someone Who Shops For You!
No More Boring Meals Or Worries About What To Eat - You Have Choices and Your Time Back!
What Do The Kidney-Friendly Meal Plans And Recipes Look Like?
WATCH THE VIDEO [Captioning is available] TO SEE THE MEAL PLAN LIVE
Here's the links to purchase this meal plan:
SO IF YOU ARE READY TO CHANGE YOUR LIFE -- CLICK ON THE BUTTON BELOW FOR THE CALORIE PLAN THAT MEETS YOUR NEEDS
[If you choose the wrong one, let me know and I can switch you to the other plan, no problem]
***** You will be taken to a sister site that will allow you to purchase and manage your meal plans *******
Meal plans are $19.99/month [Introductory price] and you lock in your price for the meal plan (until you cancel)
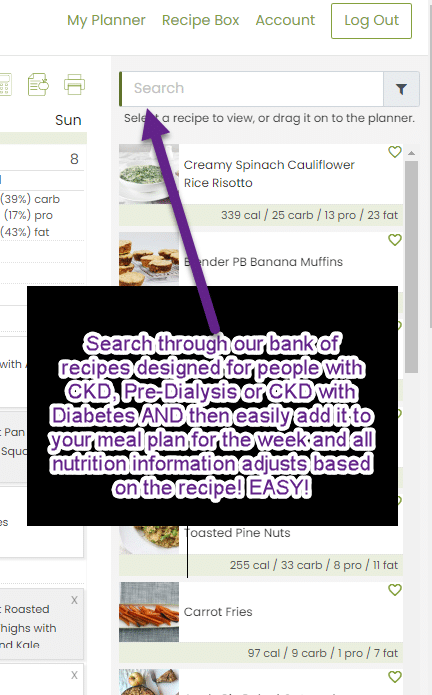
How will you know what to eat for breakfast, snacks and lunches? You get a meal pattern that gives you the flexibility of choosing from the different food types (fruits for example) and create your meals for the day. It's prebuilt and you adjust for what you need.
You won't be bored, we have new recipes every week and a variety of meals - beef, chicken, turkey, vegetarian and fish - and you can choose from over 300 recipes that were created for CKD patients with lower protein and sodium.
It is done for you but it is done in a way to help you succeed. You get to customize the food choices to make it into the way it works for you to improve your kidney health.
With these menu plans you might get some time back in your day to relax... Best of all, these are recipes that will make you healthier and keep you feeling great - as a FAMILY. These are built for 2 people BUT you can increase the servings on the recipes and it will adjust all the ingredients and you can make it for your entire CLAN!
When you get your meal plan each week, you also get an itemized grocery list for the meal plan which means you save gas from less trips to the grocery store because you have a plan to follow.
It's as simple as putting the meal together using the sheet and you are always ready to eat while keeping your diet in check!
The shopping/grocery lists are easy to take to the store, or just give to someone to shop for you. Cross out what you don't need and your shopping list for the week is ready.
At this point, I want you to stop thinking about all of the things you're having to say "No" to and think about saying "Yes". I'm not going to belabor the product - it's an easy YES!
You might be thinking about all of the things you have to limit. It's a feeling of "I can't have..." But what if we focused on the tasty foods that you can have?
What if you said "YES!"
Say YES to delicious food.
Say YES to healthier kidneys.
Say YES to these meal plans that have been lovingly and carefully designed with you in mind.
I'm saying YES!
Please Give Me INSTANT ACCESS To The Entire Pre-Dialysis Renal Diet Meal Plans, Grocery Lists, and Recipes
I understand I'll be accessing the entire Pre-Dialysis Renal Diet Meal Plans for a tiny investment of just $9.99/month when I act now!
I will receive weekly meal plans and recipes that are flexible and adjustable just for me!
For only $19.99/month digital delivery! (Only $19.99/month until you cancel)

An Unbelievable Value!
Order with confidence on 100% secure servers.
***** You will be taken to a sister site that will allow you to purchase and manage your meal plans *******

With each passing month you become more independent with your health and by following the meal plans and educating yourself you will begin to feel better both physically and emotionally.
This all encompassing program is an unbelievable value and please get started now. Why not? It's your best resource to improved kidney health!! Best wishes to your great success
How Do I Receive My Pre-Dialysis Meal Plan?
- Go to our sister site where the meal plans are housed, pay for your meal plan, and you will set up a login and password
- You will get emails from the site reminding you of your meals for the week and to login and grab a new plan
- Once Access Has Been Established Your Meal Plans Will Be Accessible For Download & Printing
- You will receive a series of emails with information on how to adjust, change and use your meal plans
Money-Back Satisfaction Guarantee
Your success is important to me...
If you aren't 100% happy just let me know within 30 days....
Mathea Ford RDN/LD
I understand that it seems like an overwhelming task just to plan your meals - NO MORE!
If you don't sign up, you will go back to struggling every day and wondering if what you are eating is the right thing for you.
You may even progress to Stage 3 or 4 or even dialysis much more quickly than if you did not follow a well planned renal diet.
You don't want to continue to spin your wheels and not move in the right direction to have a better quality of life, do you?
I certainly don't want you to!
P. S. If you could do one thing to make your days a little easier and your health better in the same actions, this would be it! You can save time by having well designed meals laid out for you, grocery lists that include all the things that you need (in case someone else does the shopping), and a whole lot of peace of mind that you are on the right path to healing your kidneys... Get the pre-dialysis diet meal plans and get started now!

FAQs
Q. How do I know how many calories to choose?
A. Your recommended calorie intake depends on various factors, like age and activity level. Most women need 1,500–2,000 daily calories to maintain their weight. Most men need 2,000–3,000 calories. Eating fewer can lead to weight loss. Any meal plan can be adjusted to increase or decrease calories per day by adding side dishes or removing recipes. Speak with your dietitian to get more specific calories for your personal needs. If you want to switch to the other meal plan, please contact me and I will switch your plan.
Q. What if I don't eat a certain food?
A. The food plans are completely customizable. If you don't like chicken or onions, no worries. There will still be plenty of options available for you. You can select a different recipe for you.
Q. Will you fix my meal plan for me or provide me with estimated calories, etc?
- I don't personally tailor the meal plan for you based on your own preferences or needs - you will need to adjust it yourself
- I don't meet with your or provide ANY nutritional advice related to your labs or current medications or needs - due to liability issues, I cannot do that!
Q. Is this the right program for me?
A. We have three different menu plans.
- Pre-Dialysis Menu Plan. (The menu plan on this page.) Choose this option if you want a kidney healthy diet, are not on dialysis, and do not have diabetes. Even if you are pre-diabetic, this is the menu plan for you as eating a kidney healthy diet is also great for your blood sugar.
- Renal Diabetic Menu Plan. This is for you if you are diabetic, want a healthy renal diet, and are not on dialysis. It is a more restrictive plan that should only be used by diabetic patients.
- Dialysis Menu Plan. Only choose the dialysis menu plan if you are currently on dialysis.
Q. I'm not sure about this program. Is it easy to cancel?
A. Of course! All you have to do is log into your account and you can cancel in there at any time. If you need help, simply contact us.











